Introduction
Understanding the nuances of T waves in electrocardiograms (ECGs) is essential for healthcare professionals, as these signals offer critical insights into cardiac health. Peaked T waves, in particular, frequently indicate serious underlying conditions such as hyperkalemia and myocardial ischemia. This article explores the fundamental techniques for mastering the analysis of peaked T waves, examining their clinical implications and the advanced technology that enhances ECG interpretation. Clinicians must accurately identify and respond to these vital changes in cardiac signals to improve patient outcomes.
Define T Waves in ECG: Characteristics and Importance
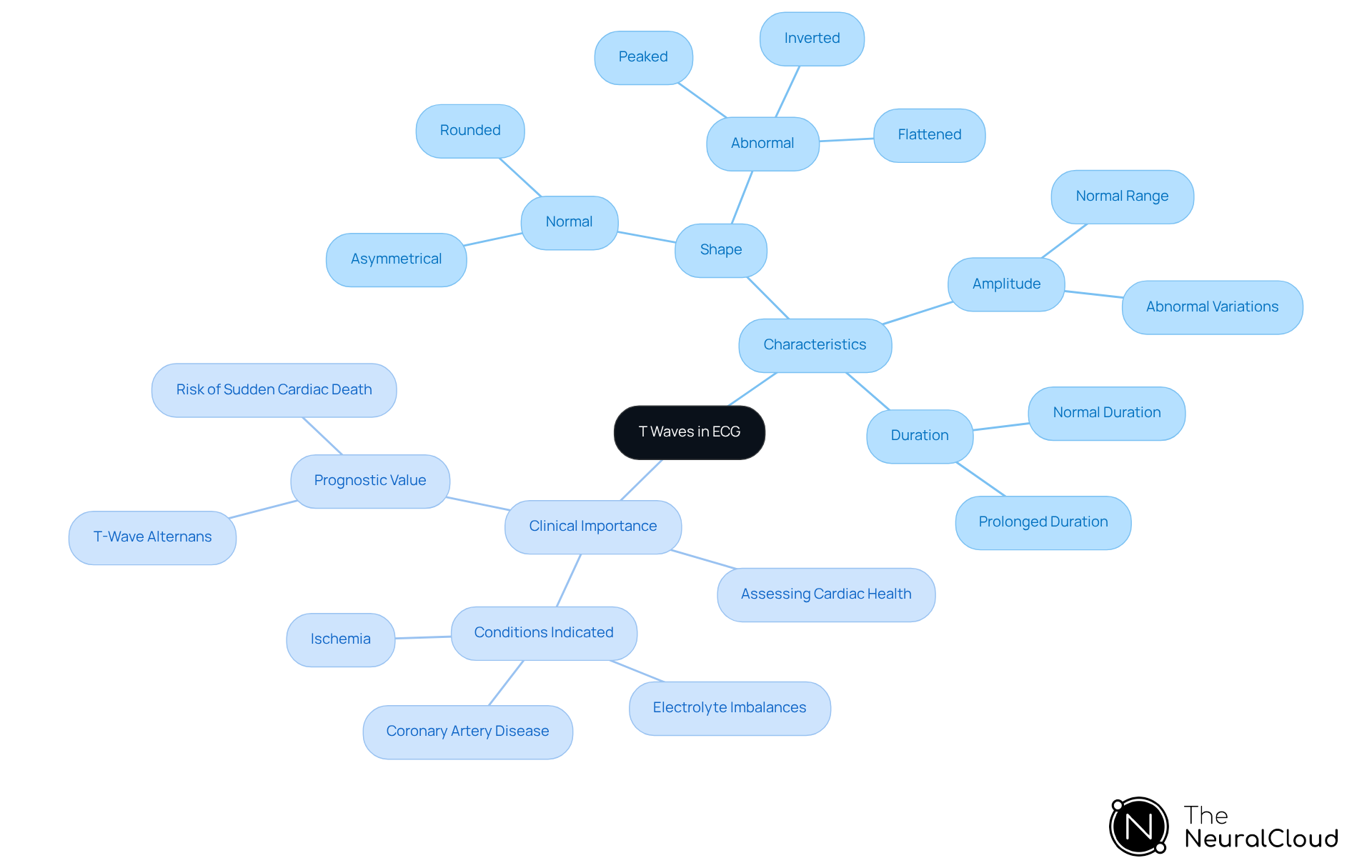
are a fundamental aspect of the electrocardiogram (ECG), signifying the repolarization of the ventricles following contraction. Typically, they manifest as a positive deflection after the QRS complex. The characteristics of T waves—shape, amplitude, and duration—can fluctuate based on both physiological and pathological states. Normal T wave shapes are typically asymmetrical and rounded, whereas abnormalities may manifest as a peaked T wave, inverted, or flattened forms. Understanding these variations is crucial for clinicians, as they play a vital role in assessing and identifying potential issues such as ischemia or arrhythmias.
ECG analysis software, a sophisticated automated ECG analysis platform from Neural Cloud Solutions, enhances the interpretation of ECGs by offering detailed insights even in recordings with considerable noise and artifacts. Its advanced noise filtering features enable the swift separation of ECG signals, ensuring that essential data is not obscured by baseline drift or muscle artifacts. This is especially significant when examining T waves, as their shape can act as a predictive indicator for major adverse cardiovascular occurrences (MACE), particularly in individuals with heart disease.
Research indicates that T wave abnormalities can serve as a prognostic marker for MACE, particularly in patients with heart conditions. For example, T-wave alternans (TWA) has been associated with heightened vulnerability to sudden cardiac death, emphasizing the significance of T wave analysis in risk assessment. A case study on T-wave analysis during 24-hour Holter ECG monitoring demonstrated that T-wave characteristics, including onsets, offsets, and time-series intervals, could independently predict MACE in patients with myocardial ischemia, underscoring their clinical relevance.
Furthermore, irregularities in the T-wave, particularly peaked forms, can signify underlying cardiac issues such as coronary artery disease or myocardial ischemia. The ability to accurately interpret these changes is essential for timely intervention and improved patient outcomes. With advanced ECG technology, health tech developers can incorporate enhanced analysis and improved clarity into their systems, ensuring that T waves are not just a part of the ECG but essential indicators of cardiac health that necessitate thorough analysis and comprehension.
Explore Peaked T Waves: Clinical Implications and Diagnostic Relevance
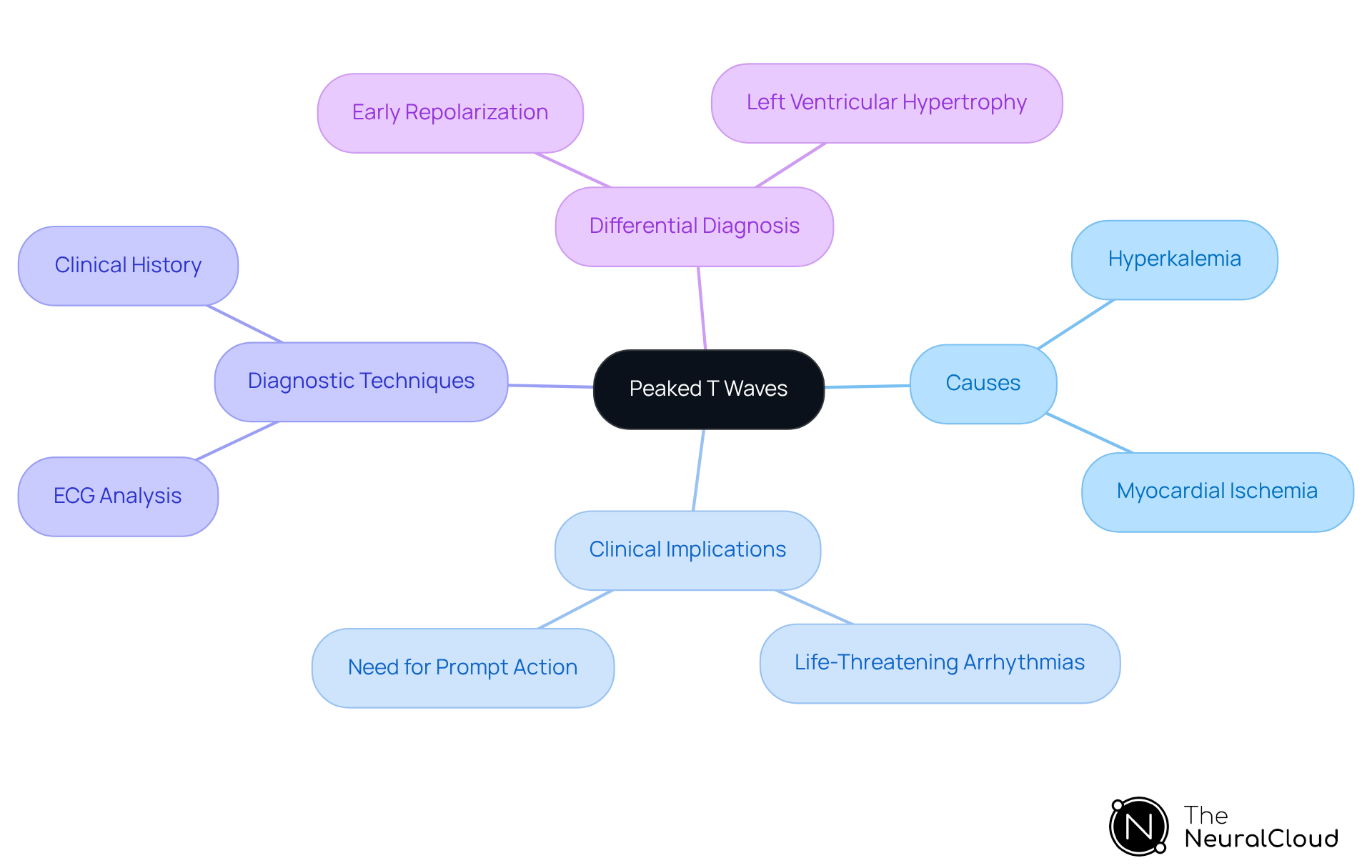
Peaked T wave forms are characterized by their tall, narrow, and symmetric morphology on the ECG. Clinically, these patterns are most frequently linked to hyperkalemia, defined as a serum potassium level exceeding 5.5 mEq/L, which can result in life-threatening arrhythmias if not swiftly addressed. Recognized as a primary reason for cardiac arrest, these patterns can indicate myocardial injury, particularly in the context of ST-elevation myocardial infarction (STEMI). Hyperacute T forms, which are broad-based and symmetrical, often precede ST-segment elevation and are critical for the early diagnosis of acute ischemia. Recognizing these patterns is essential for healthcare professionals, as they inform immediate interventions and guide further diagnostic testing.
A systematic approach, integrating a comprehensive clinical history and physical examination, is vital for the swift identification and management of conditions linked to the ECG changes, such as ischemic heart disease. The technology enhances analysis by effectively filtering noise and improving signal quality. This capability allows for the interpretation of lengthy Holter, 1-Lead, and patch monitor recordings. In emergency settings, where timely decision-making can significantly impact patient outcomes, this feature is particularly beneficial. Clinicians should also consider the differential diagnoses, including conditions like early repolarization and left ventricular hypertrophy, to avoid misinterpretation.
Analyze Peaked T Waves: Step-by-Step ECG Interpretation Techniques
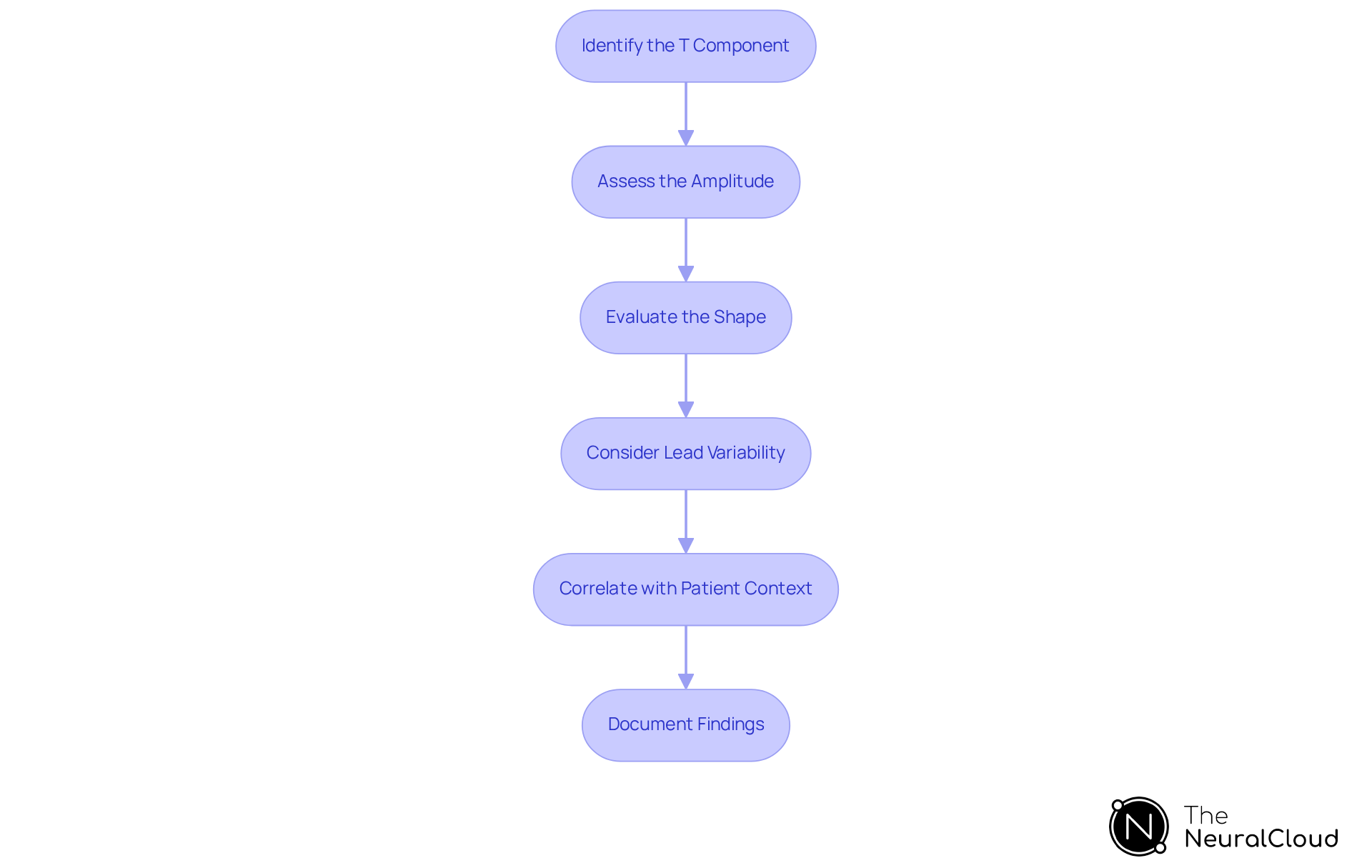
To effectively analyze T waves, follow these steps:
- Identify the T Component: Begin by locating the T component that follows the QRS complex in the ECG tracing. It is essential to view the correct leads, as T morphology can vary across different leads, ensuring both accuracy and efficiency compared to traditional methods.
- Assess the Amplitude: Measure the amplitude. Peaked T wave forms typically exceed 5 mm in limb leads and 10 mm in precordial leads, indicating potential cardiac issues. The hazard ratio for positive T patterns as a predictor of mortality is 6.76, underscoring the clinical significance of T-amplitude, facilitating rapid identification of critical changes.
- Evaluate the Shape: Examine the T wave for symmetry and narrowness. Peaked T wave forms should appear sharp and well-defined, without broadening or flattening, which may suggest different pathologies. Hyperacute T wave forms, for example, are characterized by being high-peaked, sharp, and broadened at the base, indicating serious conditions that enable accurate shape analysis, streamlining the process beyond traditional methods.
- Consider Lead Variability: Analyze the T shape across multiple leads to determine whether the peaked morphology is localized or diffuse. This analysis can provide insights into underlying pathology, such as myocardial ischemia. Comparing T-wave changes with previous ECGs is crucial for assessing their significance. MaxYield™ allows for seamless integration of historical data, enriching your analysis by providing context that traditional methods may overlook.
- Correlate with Clinical Findings: Integrate your findings with the patient's medical history and other ECG changes, such as ST segment elevation or QRS widening, to form a comprehensive assessment. For instance, hyperacute T waves may suggest acute coronary syndrome and should be evaluated alongside other medical signs. As Dr. Vernon R. Stanley emphasizes, recognizing these changes is vital in the early stages of cardiac events. MaxYield™ aids in correlating these findings by offering detailed insights, supporting informed medical decision-making.
- Document Findings: Record your observations and any relevant implications, ensuring effective communication with the healthcare team. This documentation is essential for ongoing patient management and for guiding future clinical decisions. With MaxYield™, documentation becomes streamlined, facilitating efficient communication of critical insights.
By following these steps and utilizing the capabilities of MaxYield™, healthcare professionals can enhance their ECG interpretation skills, leading to more accurate diagnoses and improved patient outcomes.
Integrate Advanced Technology: Enhancing ECG Analysis with AI Solutions
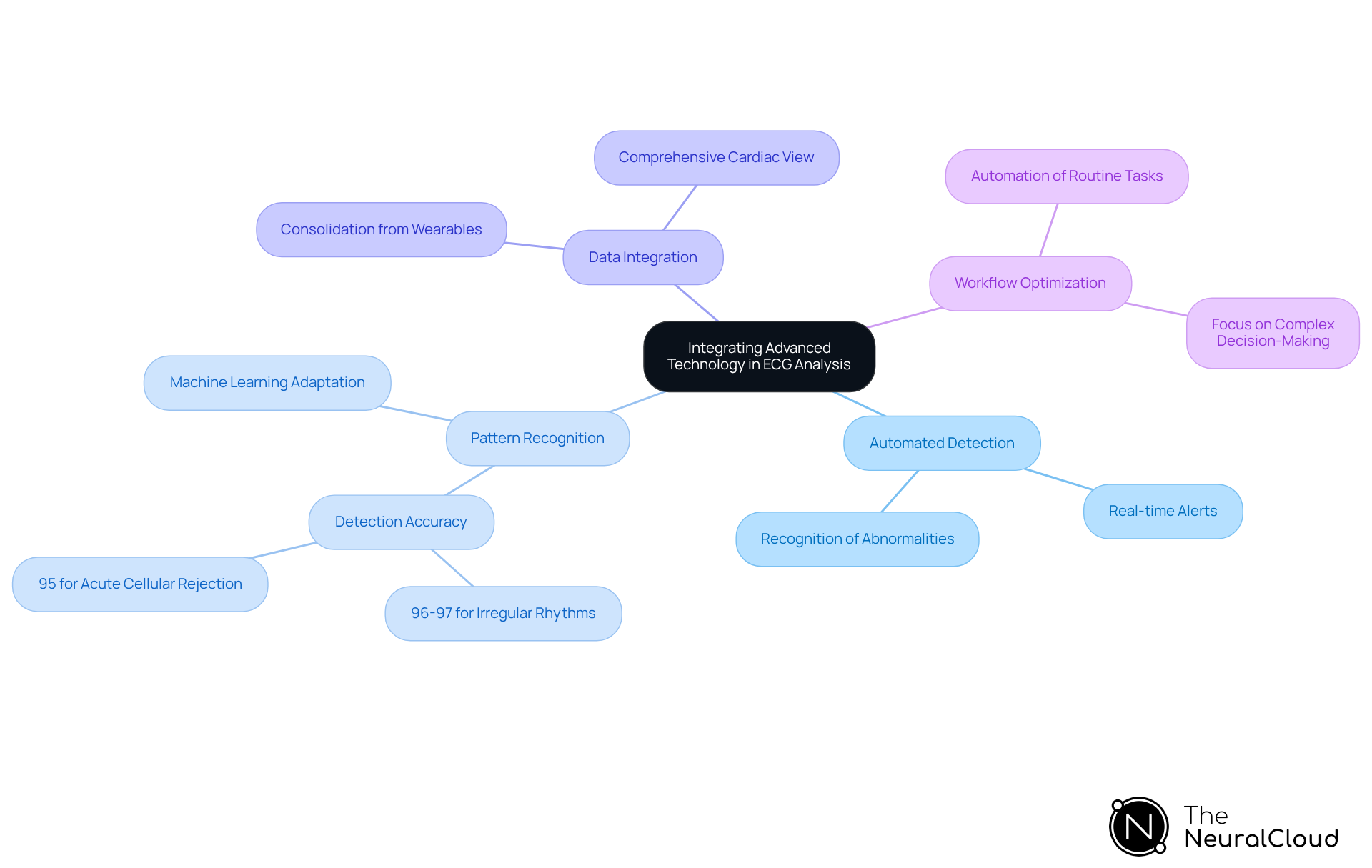
Incorporating advanced technology, particularly artificial intelligence (AI), into ECG analysis significantly enhances the identification and understanding of the peaked T wave forms, uncovering patterns that may escape human observers. Key advancements include:
- Automated Detection: AI systems are trained to recognize peaked T waves and other abnormalities in real-time, providing immediate alerts to clinicians, which is crucial for timely interventions.
- Pattern Recognition: AI algorithms are used to refine diagnostic accuracy, adapting to emerging patterns and improving over time. For instance, AI algorithms have demonstrated a detection accuracy of 96-97% in identifying irregular heart rhythms, underscoring their reliability in medical settings.
- Data Integration: AI consolidates data from various sources, including wearable devices and traditional ECG machines, offering a comprehensive view of a patient's cardiac health. This holistic approach enhances the ability to detect subtle changes in ECG readings.
- Workflow Optimization: By automating routine tasks, AI allows healthcare professionals to concentrate on complex decision-making and patient care, ultimately boosting operational efficiency.
The platform exemplifies this integration, providing tools that enhance analysis and streamline clinical workflows. This platform not only accelerates the speed of analysis but also improves accuracy, enabling healthcare providers to identify cardiac events with greater confidence.
Conclusion
Understanding and mastering the analysis of peaked T waves in ECG is crucial for healthcare professionals aiming to enhance patient outcomes. T waves serve as vital indicators of cardiac repolarization, playing a significant role in diagnosing various cardiac conditions. By focusing on the characteristics of T waves, particularly the peaked forms, clinicians can identify critical health risks, such as hyperkalemia and myocardial ischemia, which fosters timely intervention and improved patient care.
Key insights discussed include:
- A systematic approach to ECG interpretation
- The clinical implications of abnormal T wave morphology
- The integration of advanced technology like AI in enhancing diagnostic accuracy
The MaxYield™ platform streamlines the analysis process, ensuring that critical data is captured and interpreted effectively. This significantly impacts clinical decision-making, empowering healthcare providers to make informed choices that could save lives.
In summary, mastering peaked T waves in ECG analysis is not merely an academic exercise; it is a vital skill with the potential to transform patient management. As cardiology evolves with the incorporation of AI and automated systems, embracing these advancements is essential. Clinicians are encouraged to leverage these tools to enhance their diagnostic capabilities, ensuring they remain at the forefront of cardiac care and ultimately improve patient health outcomes.
Frequently Asked Questions
What do T waves in an ECG signify?
T waves in an ECG signify the repolarization of the ventricles following contraction.
How do normal T waves typically appear?
Normal T waves typically appear as a positive deflection after the QRS complex and are usually asymmetrical and rounded.
What variations can occur in T wave characteristics?
T wave characteristics, such as shape, amplitude, and duration, can vary based on physiological and pathological states, leading to abnormalities such as peaked, inverted, or flattened T waves.
Why is it important to understand T wave variations?
Understanding T wave variations is crucial for clinicians as they play a vital role in assessing cardiac health and identifying potential issues like ischemia or electrolyte imbalances.
How does MaxYield™ enhance the interpretation of T waves?
MaxYield™ enhances the interpretation of T waves by providing detailed insights and advanced noise filtering features, allowing for the swift separation of ECG signals from artifacts and ensuring essential data is visible.
What is the significance of T-wave morphology in risk assessment?
T-wave morphology can serve as a prognostic marker for major adverse cardiovascular occurrences (MACE), particularly in patients with myocardial infarction, indicating the potential for heightened vulnerability to sudden cardiac death.
Can T-wave characteristics predict major adverse cardiovascular events?
Yes, T-wave characteristics, including onsets, offsets, and time-series intervals, have been shown to independently predict MACE in patients with myocardial ischemia.
What underlying cardiac issues can peaked T waves indicate?
Peaked T waves can signify underlying cardiac issues such as coronary artery disease or myocardial ischemia.
How can health tech developers utilize MaxYield™?
Health tech developers can use MaxYield™ to incorporate automated labeling and improved clarity into ECG analysis processes, ensuring thorough analysis of T signals as essential indicators of cardiac health.
List of Sources
- Define T Waves in ECG: Characteristics and Importance
- powerfulmedical.com (https://powerfulmedical.com/blog/hyperacute-t-waves)
- mdpi.com (https://mdpi.com/2075-1729/13/5/1155)
- academic.oup.com (https://academic.oup.com/eurheartj/article/45/Supplement_1/ehae666.3009/7837056)
- patientcareonline.com (https://patientcareonline.com/view/t-wave-inversions-sorting-through-causes)
- Explore Peaked T Waves: Clinical Implications and Diagnostic Relevance
- ECG Diagnosis: Hyperacute T Waves - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC4500486)
- clinician.com (https://clinician.com/blogs/clinicians/understanding-peaked-t-waves)
- Analyze Peaked T Waves: Step-by-Step ECG Interpretation Techniques
- ecgcourse.com (https://ecgcourse.com/answer-key-differential-diagnosis-for-peaking-t-waves?srsltid=AfmBOor1CcfaARL3cgcRD95RiuZKHRJ3Yqj84g-aDj43w7t70U4vnFIN)
- amboss.com (https://amboss.com/us/knowledge/ecg)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC6932581)
- Integrate Advanced Technology: Enhancing ECG Analysis with AI Solutions
- New study suggests ECG-AI can detect cardiovascular disease risks sooner - Mayo Clinic News Network (https://newsnetwork.mayoclinic.org/discussion/new-study-suggests-ecg-ai-can-detect-cardiovascular-disease-risks-sooner)
- news-medical.net (https://news-medical.net/news/20250721/AI-powered-ECG-model-outperforms-doctors-in-detecting-hidden-heart-disease.aspx)
- Current and Future Use of Artificial Intelligence in Electrocardiography - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10145690)
- Investigating the Efficacy of AI-Powered Innovations in ECG Analysis and Continuous Heart Monitoring: A Comprehensive Narrative Review (https://cureus.com/articles/376607-investigating-the-efficacy-of-ai-powered-innovations-in-ecg-analysis-and-continuous-heart-monitoring-a-comprehensive-narrative-review)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S2001037024004550)