Introduction
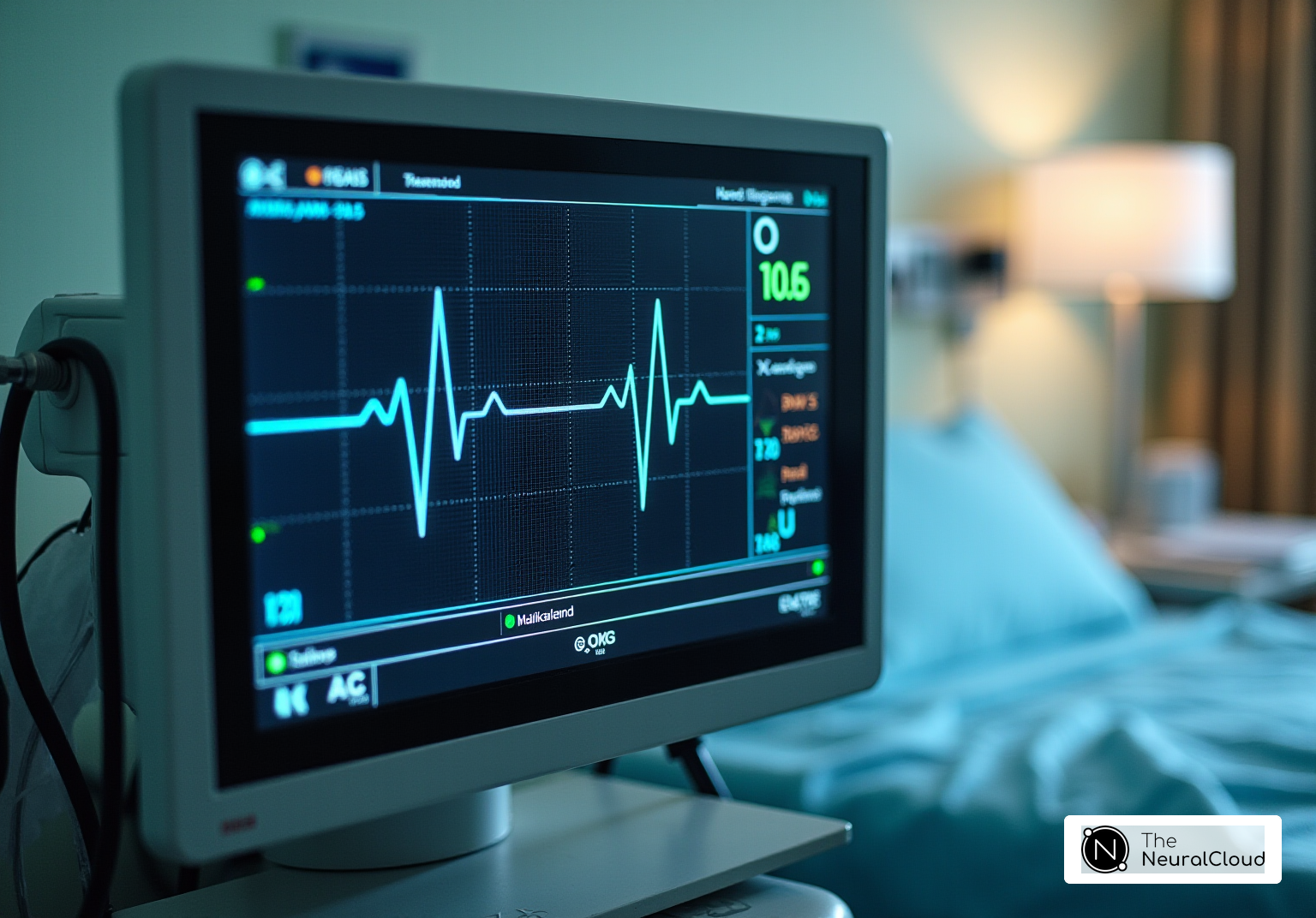
Understanding the intricacies of first-degree heart block is essential for clinicians navigating the complexities of cardiac health. This condition, characterized by a prolonged PR interval on an ECG, presents unique challenges in diagnosis and management that can significantly impact patient care.
The evolution of healthcare technology introduces tools like Neural Cloud Solutions' MaxYield™ platform, which revolutionizes ECG analysis by offering enhanced accuracy and efficiency.
Practitioners must effectively master the interpretation of first-degree heart block to ensure optimal outcomes for their patients.
Define First-Degree Heart Block: Key Characteristics and Mechanisms
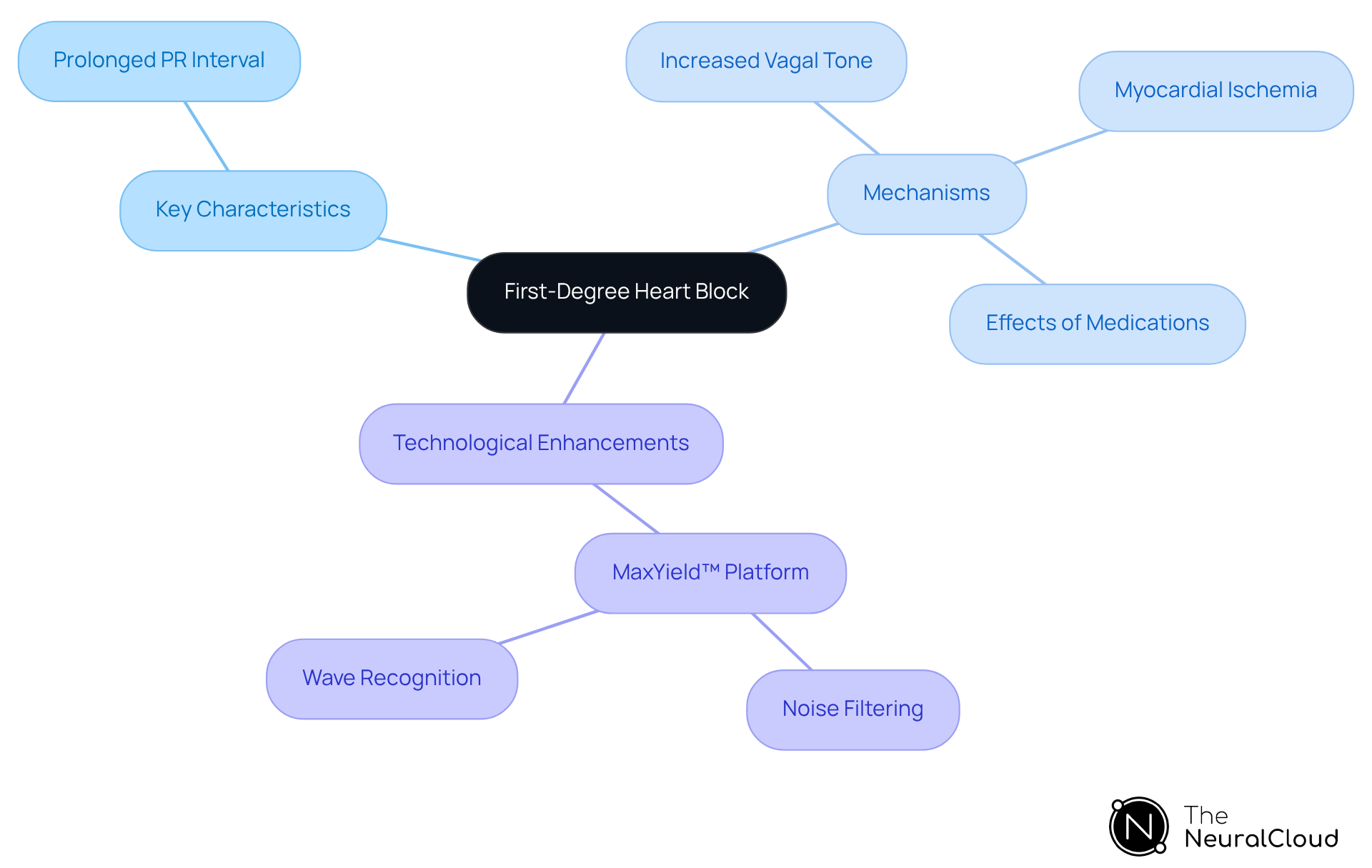
First-degree heart block, also known as first-degree atrioventricular (AV) obstruction, is characterized by a prolonged PR interval exceeding 200 milliseconds. This condition signifies a delay in the conduction of electrical impulses from the atria to the ventricles, occurring without any missed beats. The underlying mechanism involves a slowing of conduction through the AV node, which may be attributed to factors such as increased vagal tone, myocardial ischemia, or the effects of medications. Understanding these characteristics is crucial for clinicians to distinguish first-degree heart block from other types of AV blocks and to evaluate its clinical significance.
Integrating Neural Cloud Solutions' technology enhances the efficiency of ECG analysis for clinicians. This advanced system employs noise filtering and wave recognition techniques, enabling the rapid isolation and labeling of critical data, even in recordings that exhibit high levels of noise and artifact. Such capabilities not only facilitate the precise identification of heart issues through ECG analysis, but also bolster confident clinical decision-making by providing accurate information.
By automating the evaluation process, the system addresses common challenges in ECG interpretation, including physiological variability and signal artifacts. This ultimately improves diagnostic accuracy, providing healthcare professionals with the tools needed to improve patient care.
Explore Causes and Risk Factors of First-Degree Heart Block
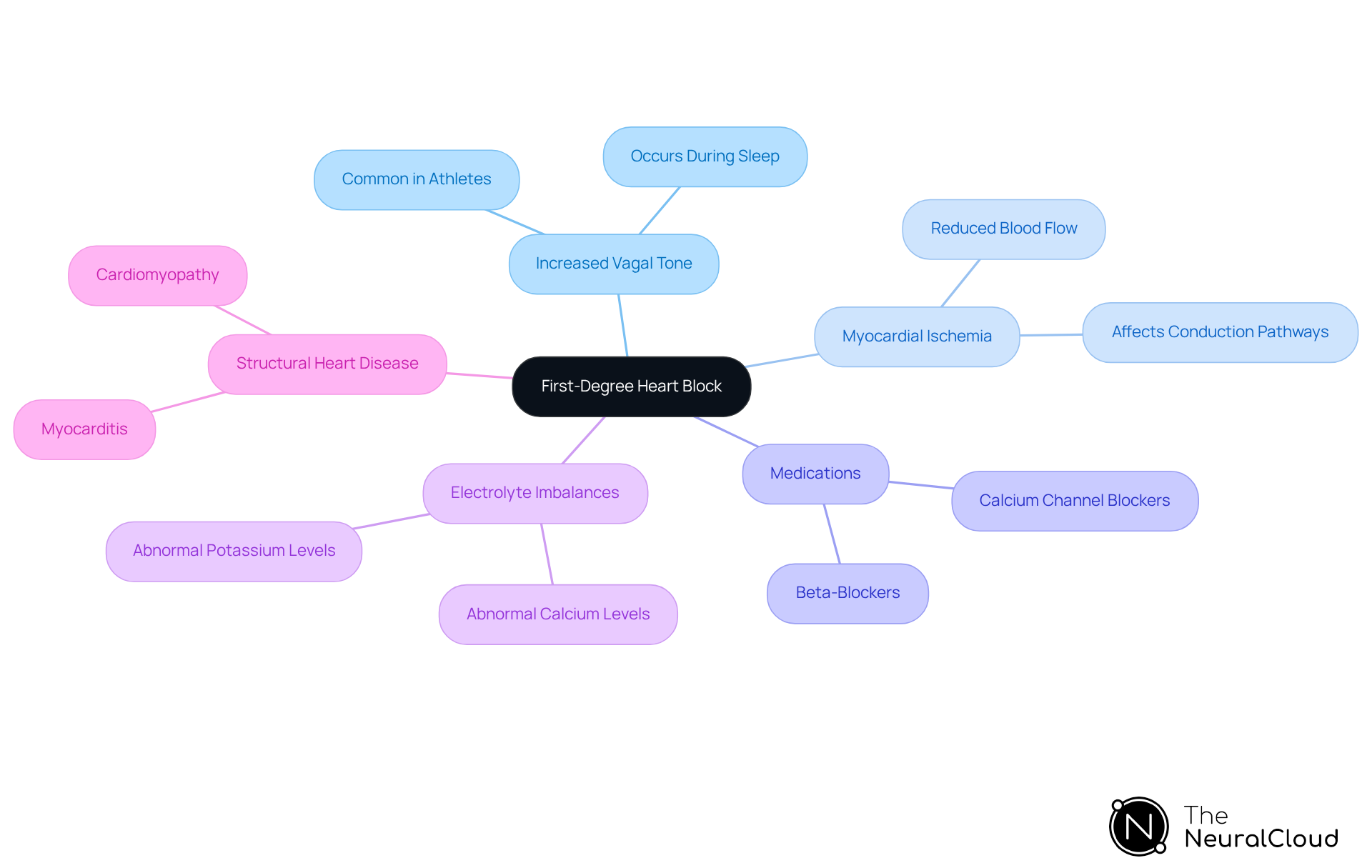
First-degree heart block can arise from various causes, including:
- Increased Vagal Tone: Often seen in athletes or during sleep, leading to a natural slowing of heart rate.
- Myocardial Ischemia: Reduced blood flow to the heart muscle can result in issues by affecting conduction pathways.
- Medications: Certain drugs, such as beta-blockers or calcium channel blockers, can prolong the PR interval, potentially indicated by a change in heart rhythm.
- Electrolyte imbalances: Abnormal levels of potassium or calcium can disrupt normal electrical conduction, which may be observed on an ECG.
- Structural Heart Disease: Conditions like myocarditis or cardiomyopathy may also contribute to abnormalities observed in a patient's heart function.
Understanding these causes is crucial for clinicians to assess the patient's overall health and potential need for further intervention. By utilizing the latest technology, health tech developers can automate ECG analysis, improving the detection of heart block through advanced algorithms and comprehensive insights from noisy recordings. This integration simplifies the diagnostic process, aiding clinicians in making informed choices based on precise and dependable data.
Interpret ECG Findings: Diagnosing First-Degree Heart Block
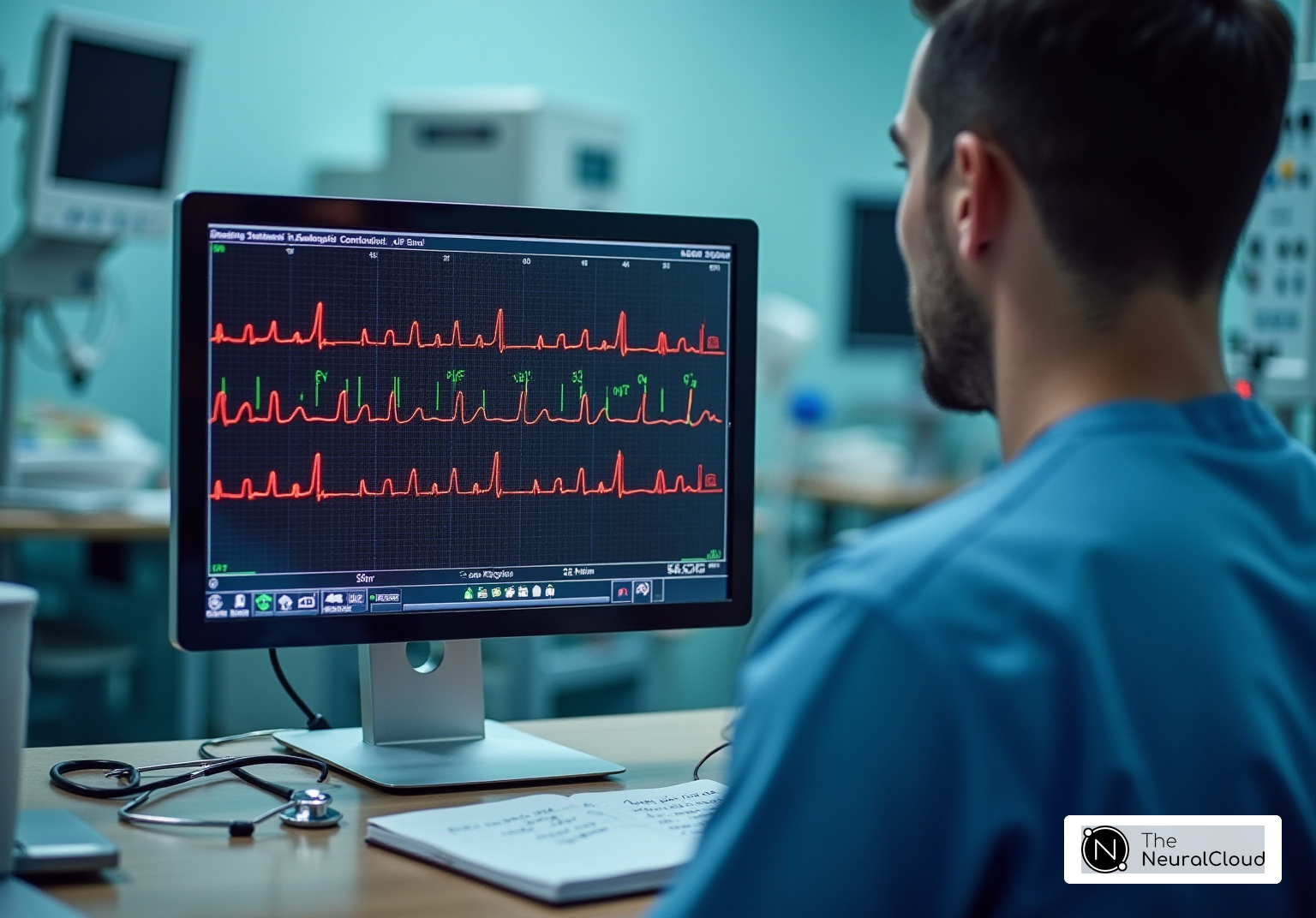
To diagnose first-degree heart block, clinicians must carefully analyze the ECG for key findings, utilizing the capabilities of technology for enhanced accuracy and efficiency.
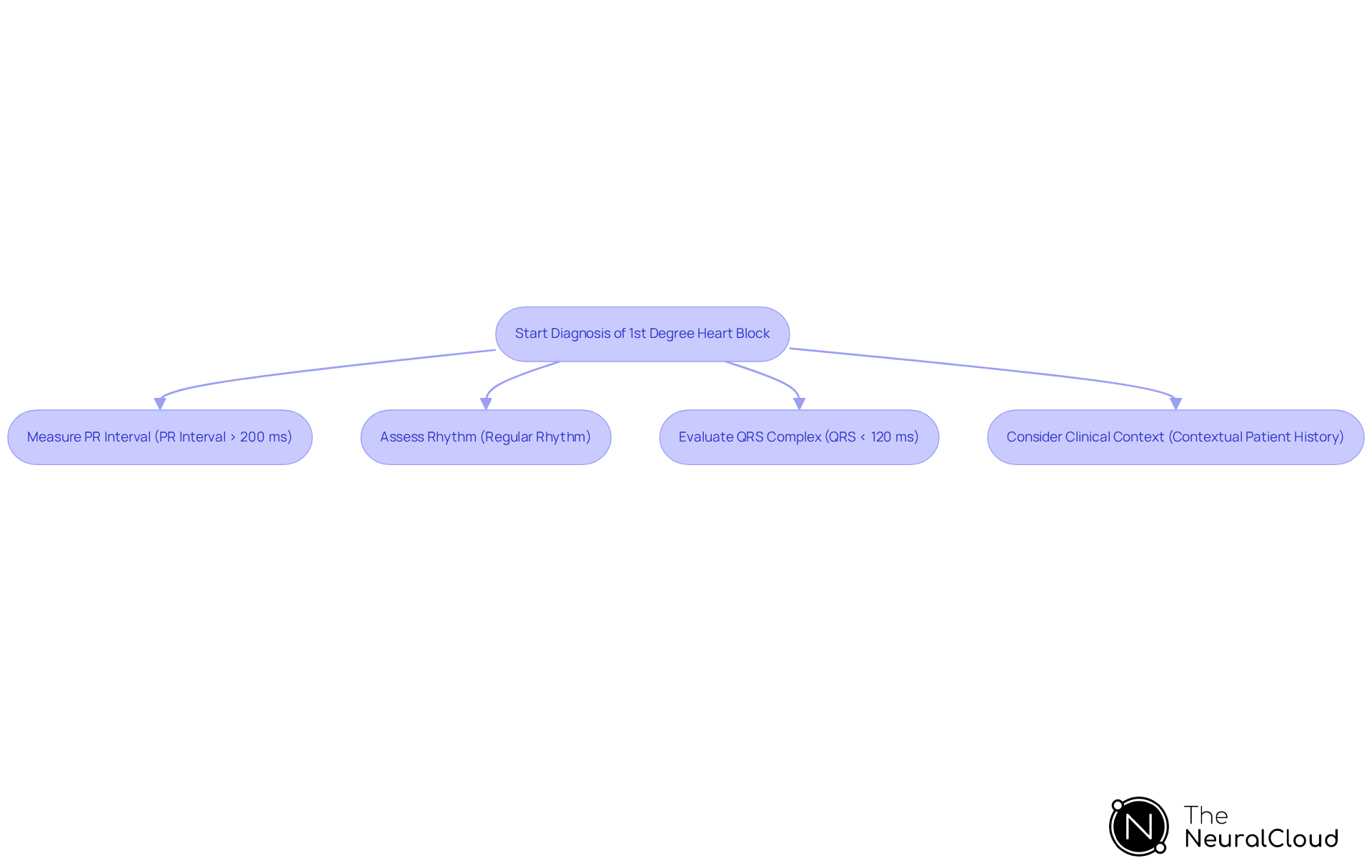
- PR Interval: Measure the distance from the beginning of the P wave to the beginning of the QRS complex. A consistent PR interval greater than 200 milliseconds indicates a diagnosis on the ECG. The system automates this measurement, ensuring precision in identifying heart block through its beat-by-beat analysis.
- Rhythm: The rhythm should be regular, with each P wave followed by a QRS complex, indicating that all atrial impulses are conducted to the ventricles. This tool assists in visualizing the relationship clearly in a digital format, reducing noise and enhancing waveform clarity, which is crucial for accurate interpretation.
- QRS Duration: The width of the QRS complex should be normal (less than 120 milliseconds) unless there is an underlying bundle branch block. With this tool, clinicians can quickly evaluate QRS width and detect any irregularities, enhancing the diagnostic process.
- Clinical Context: Always interpret the findings of the ECG in conjunction with the patient's clinical history and symptoms. For instance, asymptomatic patients may not require treatment, while those with symptoms may need further evaluation. This system facilitates this contextual examination by offering extensive insights into each heartbeat, enabling informed clinical choices and converting ECG data into practical insights.
By mastering these interpretation skills and utilizing advanced tools, clinicians can ensure effective and appropriate management strategies, overcoming traditional limitations in ECG analysis.
Manage First-Degree Heart Block: Treatment and Follow-Up Strategies
Management of first-degree heart block typically involves several key strategies.
- Observation: For asymptomatic patients, immediate treatment is usually unnecessary. Regular follow-up ECGs, such as the standard ECG, are recommended to monitor for any progression to higher-degree AV block. Leveraging AI platform enhances the accuracy of these follow-ups by providing real-time data and advanced noise filtering, ensuring clearer ECG readings even in challenging conditions.
- Medication Review: It is essential to evaluate and adjust any medications that may contribute to the condition, such as beta-blockers or calcium channel blockers. Incorporating a medication management system with this system facilitates real-time monitoring of patients' responses to these medications, allowing for timely adjustments.
- Patient Education: Patients should be informed about the condition, potential symptoms to watch for, and when to seek medical attention. AI-driven automation in ECG evaluation can assist in offering clearer information to patients, improving their comprehension of the condition.
- Follow-Up: Routine follow-ups are necessary to assess the patient's condition and ensure that no new symptoms develop. If symptoms such as syncope or severe bradycardia occur, further evaluation and potential intervention may be necessary. The continuous learning model of MaxYield™ ensures that each ECG analysis improves over time, effectively addressing patient needs.
By implementing these management strategies, supported by advanced innovative technology, healthcare providers can effectively monitor and support patients with first-degree heart block, ensuring optimal cardiac health.

Conclusion
Mastering the analysis of first-degree heart block ECG is crucial for effective clinical practice. This condition, characterized by a prolonged PR interval, serves as a significant indicator of electrical conduction delays between the atria and ventricles. Understanding its characteristics, causes, and management strategies equips healthcare professionals to make informed decisions and enhance patient outcomes.
Key insights into diagnosing first-degree heart block involve:
- Recognizing the significance of the PR interval
- Ensuring accurate rhythm and QRS complex assessment
- Considering the patient's clinical context
The integration of advanced technology, such as Neural Cloud Solutions' MaxYield™ platform, improves the precision of ECG interpretation and streamlines the evaluation process. This allows clinicians to concentrate on delivering optimal care.
In summary, the importance of mastering first-degree heart block ECG analysis is paramount. By adopting innovative tools and strategies, healthcare providers can significantly enhance their diagnostic capabilities and patient management. A proactive approach to monitoring and patient education will not only bolster patient understanding but also promote better health outcomes. Engaging with these practices ensures that clinicians are well-prepared to navigate the complexities of cardiac care, ultimately leading to a healthier future for their patients.
Frequently Asked Questions
What is first-degree heart block?
First-degree heart block, also known as first-degree atrioventricular (AV) obstruction, is characterized by a prolonged PR interval exceeding 200 milliseconds, indicating a delay in the conduction of electrical impulses from the atria to the ventricles without any missed beats.
What causes first-degree heart block?
The underlying mechanism of first-degree heart block involves a slowing of conduction through the AV node, which may be attributed to factors such as increased vagal tone, myocardial ischemia, or the effects of medications.
How can clinicians distinguish first-degree heart block from other types of AV blocks?
Clinicians can distinguish first-degree heart block from other types of AV blocks by recognizing the prolonged PR interval on the ECG and understanding its specific characteristics and clinical significance.
What is the role of Neural Cloud Solutions' MaxYield™ platform in ECG analysis?
The MaxYield™ platform enhances the efficiency of ECG analysis by employing noise filtering and wave recognition techniques, enabling rapid isolation and labeling of critical data, even in recordings with high levels of noise and artifact.
How does the MaxYield™ platform improve clinical decision-making?
By transforming noisy recordings into detailed insights, the MaxYield™ platform facilitates the precise identification of heart issues associated with first-degree heart block ECG, thereby bolstering confident clinical decision-making.
What challenges in ECG interpretation does the MaxYield™ platform address?
The MaxYield™ platform addresses common challenges in ECG interpretation, including physiological variability and signal artifacts, ultimately enhancing diagnostic yield and workflow efficiency for healthcare professionals.