Introduction
Identifying the nuances of ST-Elevation Myocardial Infarction (STEMI) is a lifesaving skill. However, the presence of various conditions that mimic its symptoms complicates diagnosis. For health tech developers, understanding these STEMI mimics is crucial. Misinterpretation can lead to inappropriate treatments and adverse patient outcomes. How can developers leverage advanced technologies like AI to enhance ECG analysis and improve diagnostic accuracy? This article delves into ten key STEMI mimics that every health tech developer should know. It highlights the importance of precise differentiation in clinical practice.
Neural Cloud Solutions: Advanced ECG Analysis for Identifying STEMI Mimics
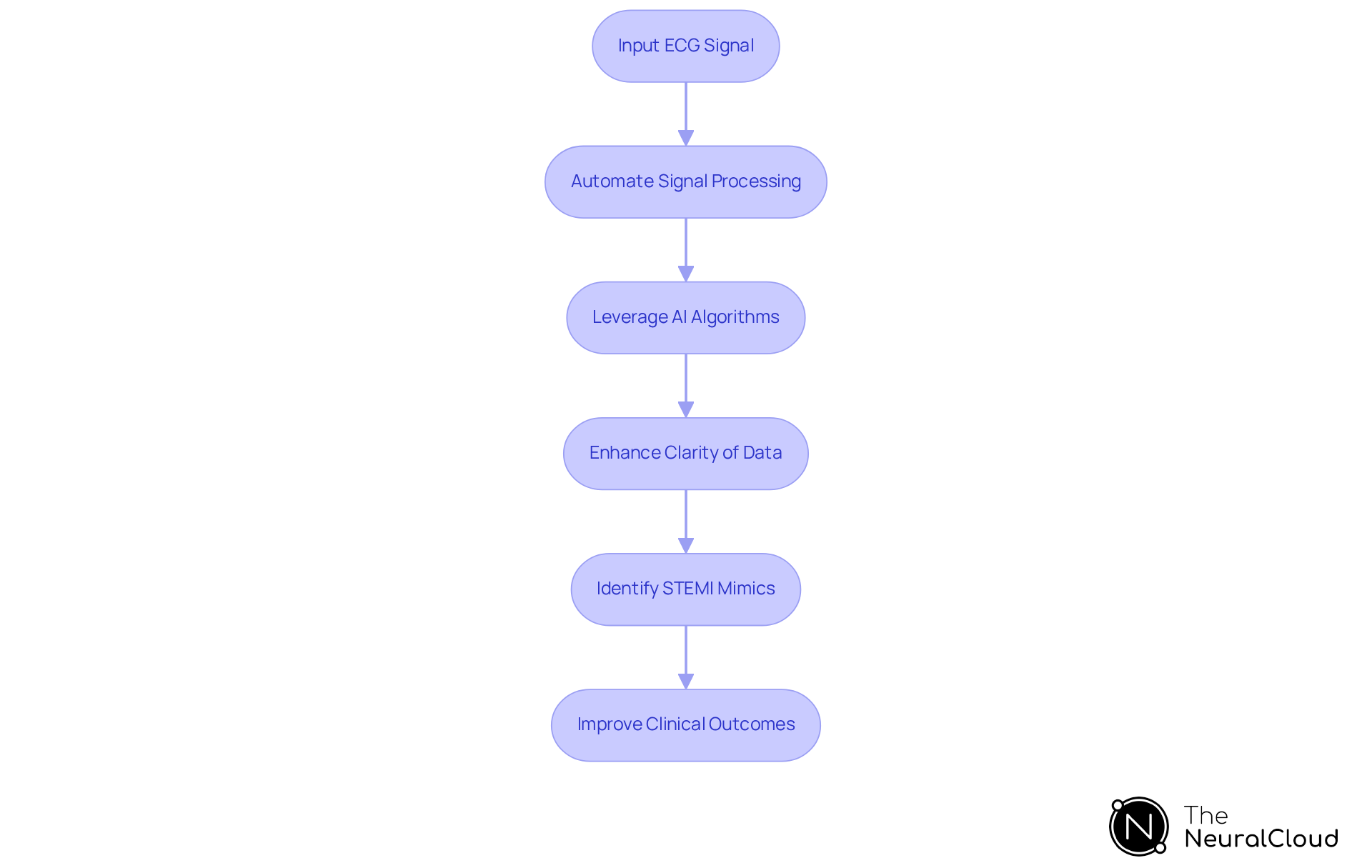
Neural Cloud Solutions addresses the challenges in ECG analysis through its platform, which provides crucial insights for identifying STEMI mimics. By automating ECG signal processing and leveraging sophisticated AI algorithms, the platform enhances the clarity of cardiac data. This advancement empowers healthcare practitioners to effectively diagnose conditions that may present similar ECG patterns.
The significance of accurate diagnosis is highlighted by cardiologists, who stress that ongoing chest pain accompanied by ECG changes should not be disregarded, even if it does not meet traditional ST-elevation MI criteria. Recent studies reveal that advanced algorithms can achieve an area under the curve (AUC) of 0.938 in detecting STEMI mimics, demonstrating its superior accuracy compared to conventional methods.
Additionally, the platform's capability to process over 200,000 heartbeats in less than five minutes facilitates rapid differentiation between myocardial infarction and other conditions, ultimately leading to better patient outcomes. As the field of AI in ECG analysis evolves in 2025, the integration of such advanced technologies becomes essential for health tech developers focused on enhancing accuracy and patient care.
Brugada Syndrome: Recognizing ECG Features to Differentiate from STEMI
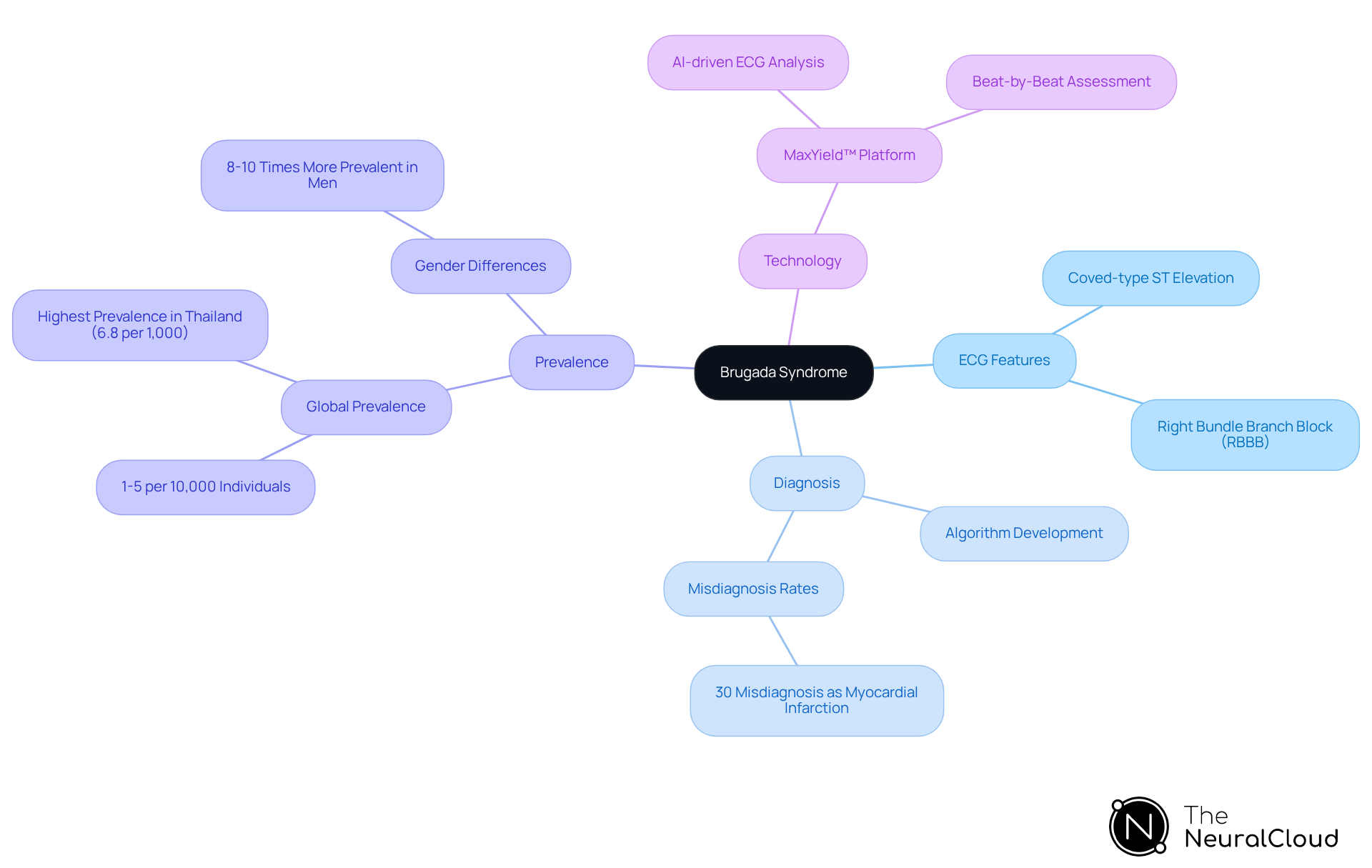
in the right precordial leads (V1-V3), which can often be mistaken for a heart attack. Developers must prioritize the identification of this specific syndrome, along with the presence of a right bundle branch block (RBBB), to improve diagnostic accuracy. Misdiagnosis can be significant; studies indicate that up to 30% of cases may be incorrectly identified as myocardial infarction. This highlights the necessity of developing algorithms capable of distinguishing between conditions.
Neural Cloud Solutions' technology plays a pivotal role in this process by leveraging artificial intelligence and a continuous learning model to analyze ECG signals amidst noise, isolating and labeling key features in every heartbeat. MaxYield™ delivers beat-by-beat analysis, providing an assessment of 200,000 heartbeats in under 5 minutes, which enhances diagnostic yield over time. Practical applications of such algorithms have demonstrated their efficiency in differentiating from these two conditions, ultimately improving outcomes for individuals.
Cardiologists emphasize that identifying the distinctive morphology of the coved-type ST elevation is essential for accurate diagnosis, as it directly influences treatment choices and safety. Additionally, Brugada Syndrome is genetically determined, with approximately 50% of familial cases exhibiting an autosomal dominant inheritance pattern. The SCN5A gene accounts for around 30% of cases, underscoring the genetic factors associated with the condition.
It is also important to note that Brugada Syndrome is 8-10 times more prevalent in men than in women, with the typical individual being young, male, and otherwise healthy. Recognizing triggers for arrhythmias, such as fever and certain medications, is crucial for health tech developers in algorithm design. Integrating MaxYield™ can enhance the clarity and efficiency of this analysis.
Left Bundle Branch Block (LBBB): Key ECG Indicators to Distinguish from STEMI
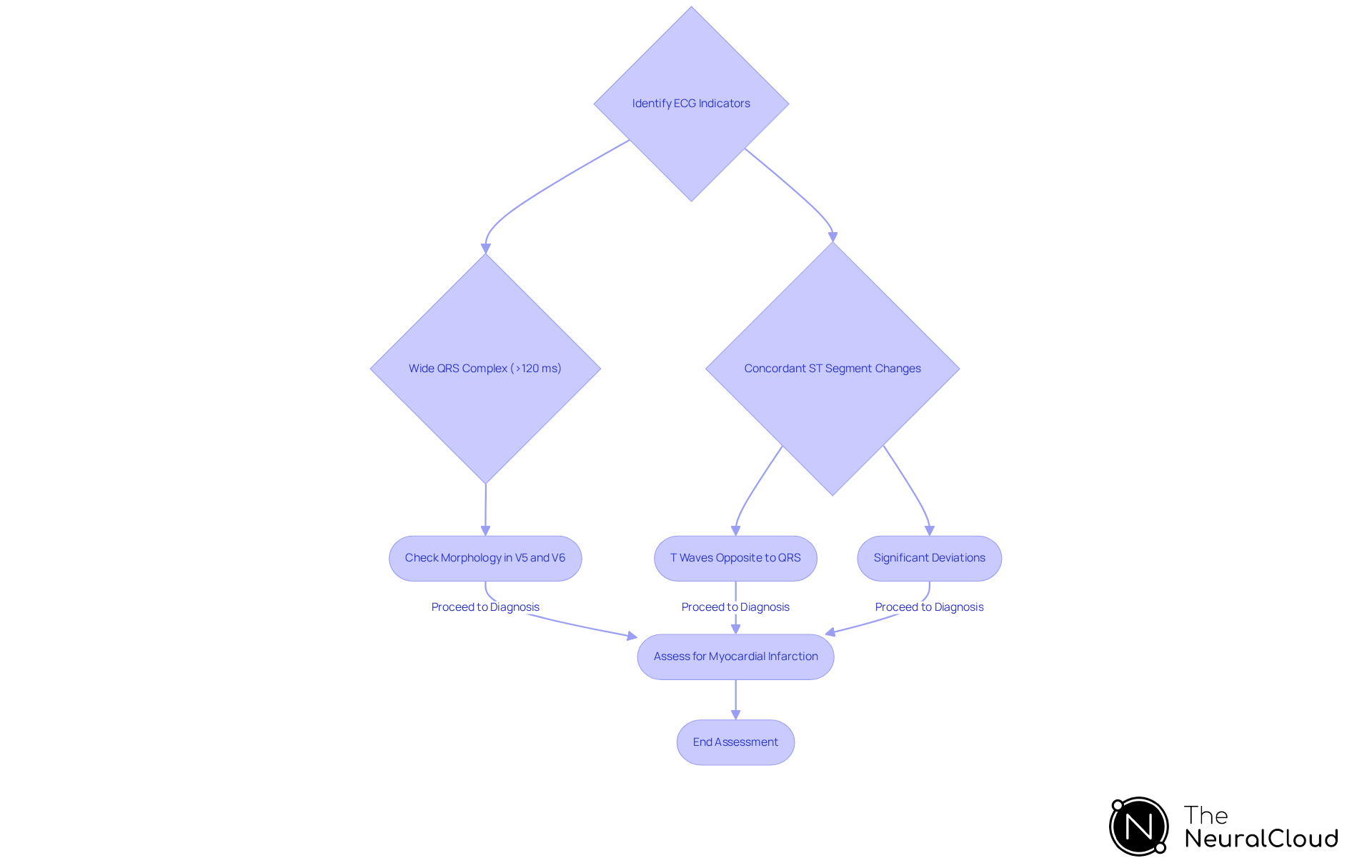
Left Bundle Branch Block (LBBB) is characterized by a wide QRS complex, typically exceeding 120 ms, and presents a distinctive 'M' shape in leads V5 and V6. This morphology can obscure the diagnosis of ST-Elevation Myocardial Infarction, particularly in anterior leads, resulting in that complicate clinical decision-making. Statistics indicate that LBBB is the second most prevalent cause of misdiagnosis, with only 1.2% of patients admitted for acute coronary syndrome also presenting with newly diagnosed LBBB. This highlights the assessment challenges encountered by healthcare professionals.
To reduce misdiagnosis, it is essential to create algorithms that accurately distinguish between LBBB and STEMI. Key indicators include the presence of concordant ST segment changes and the morphology of the QRS complex. In LBBB, T waves typically orient opposite to the QRS terminal forces; significant deviations may indicate underlying cardiac dysfunction. Advanced algorithms, such as those utilized by Neural Cloud Solutions' MaxYield™, efficiently interpret ECG data amidst interference and provide beat-by-beat analysis, enhancing accuracy in differentiating LBBB from other conditions.
Healthcare professionals emphasize the importance of recognizing these indicators, as the presence of LBBB can lead to a 2.9 times increased risk of adverse events and complicate the identification of myocardial infarction and other cardiac conditions. Understanding these subtleties is crucial for aiming to design tools that improve patient outcomes.
Pericarditis: Clinical Clues and ECG Features That Mimic STEMI
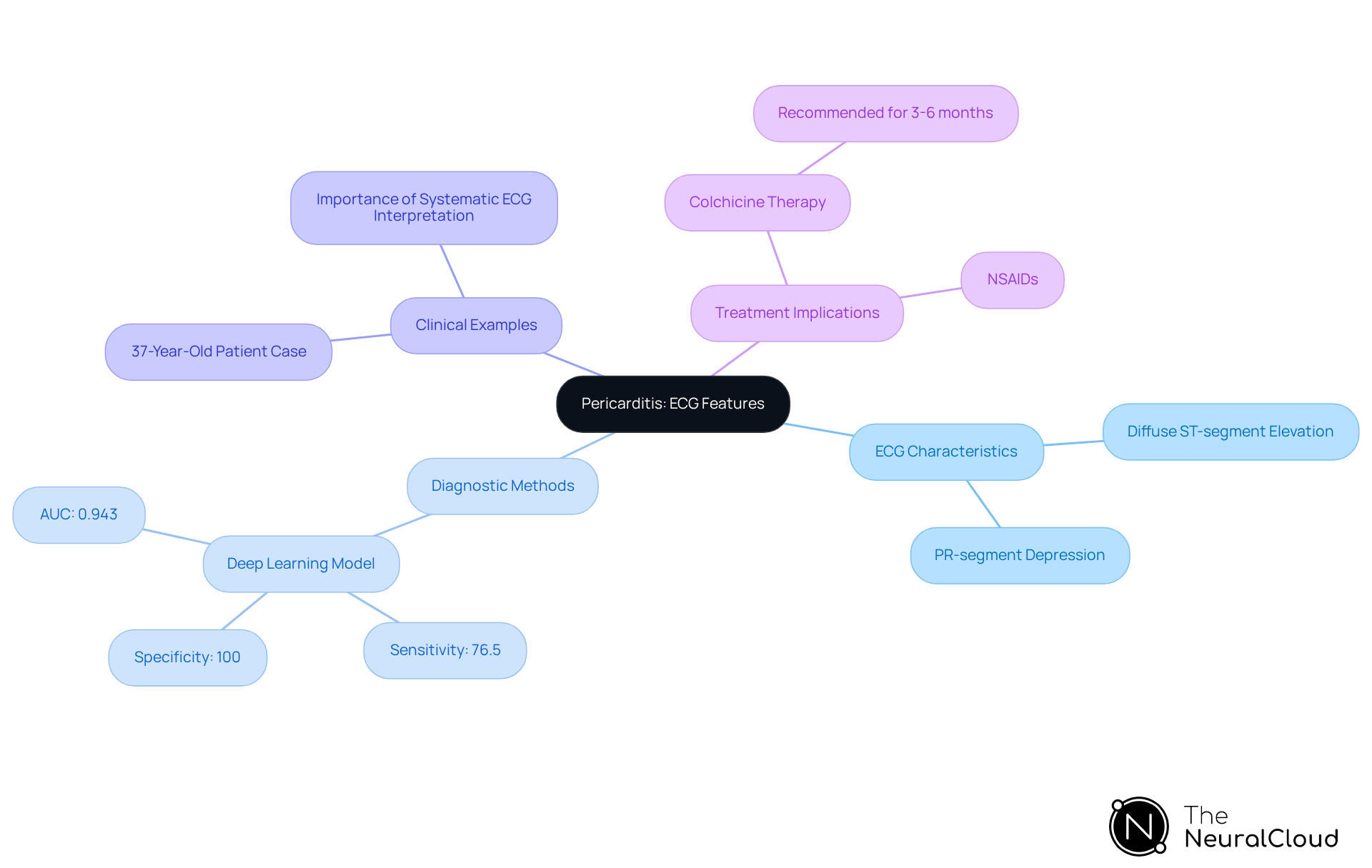
Pericarditis is characterized by diffuse ST-segment elevation across multiple leads, often accompanied by PR-segment depression. This pattern is essential for developers to identify, as it sharply contrasts with the localized ST elevation typically observed in myocardial infarction. Understanding these features is vital for creating assessment instruments that can accurately distinguish between cardiac conditions and pericarditis, including conditions like pericarditis.
In a recent study, a deep learning model demonstrated a sensitivity of 76.5% and a specificity of 100% in detecting pericarditis, outperforming traditional methods and human experts. This highlights the potential of artificial intelligence in enhancing assessment accuracy.
Real-world examples illustrate the importance of accurate diagnosis. For instance, a 37-year-old individual presenting with chest pain required a thorough examination to determine whether the ECG indicated myocardial infarction or pericarditis. By following established algorithms, clinicians were able to make an accurate diagnosis, emphasizing the necessity for ongoing education in cardiology.
Experts emphasize that recognizing the typical ECG pattern of pericarditis is crucial to differentiate it from myocardial infarction. This understanding not only facilitates accurate diagnosis but also informs treatment decisions, as timely intervention can significantly impact patient outcomes.
Integrating these insights into the development of assessment tools will enhance their effectiveness, ultimately improving patient outcomes in emergency situations.
Left Ventricular Hypertrophy (LVH): ECG Characteristics That Overlap with STEMI
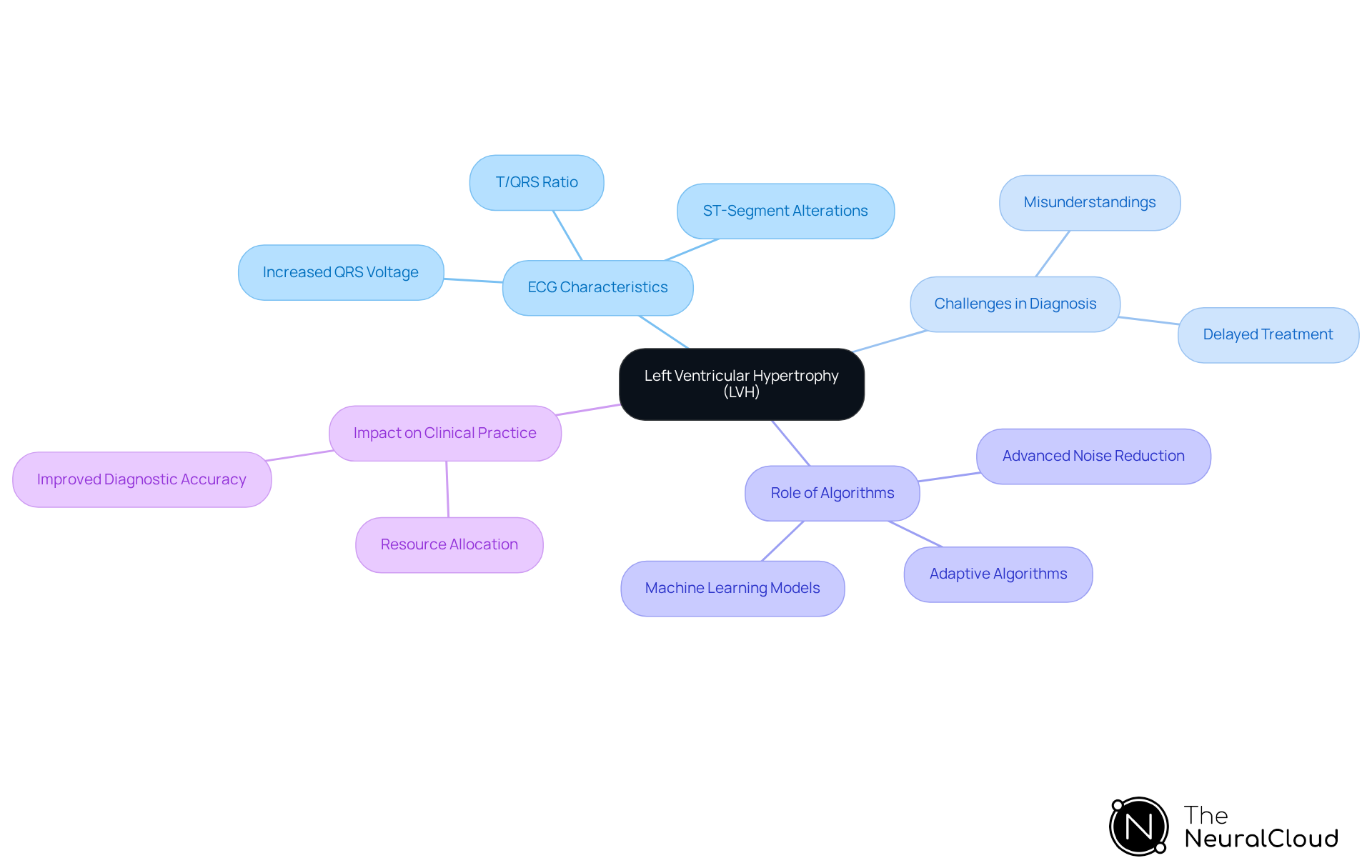
Left Ventricular Hypertrophy (LVH) is characterized by increased voltage in the QRS complexes, particularly in the left precordial leads (V1-V6). This rise can result in ST-segment alterations that closely resemble those seen in myocardial infarction, complicating the evaluation process. For instance, a T/QRS ratio greater than 0.36 suggests LVH rather than myocardial infarction, yet distinguishing between these conditions remains a challenge.
Healthcare professionals emphasize the importance of accuracy in differentiating LVH from myocardial infarction. The MaxYield™ platform from Neural Cloud Solutions features advanced noise reduction and adaptive algorithms, significantly enhancing the ability to differentiate these patterns. This platform quickly isolates relevant data from recordings with noise, directly influencing diagnostic outcomes. Consequently, developers can create algorithms that effectively distinguish between LVH and myocardial infarction.
Misunderstandings between LVH and myocardial infarction can significantly impact the accuracy of assessments. Studies indicate that the prevalence of LVH diagnosed by ECG is around 17.6%, and its presence can lead to misinterpretations that may result in misinterpretation of ST-segment elevation. This misinterpretation potentially results in delayed treatment for patients experiencing acute coronary events. Therefore, it is crucial for developers to focus on creating algorithms that accurately differentiate these overlapping ECG patterns, thereby improving patient care and resource allocation in emergency settings.
Incorporating artificial intelligence into ECG interpretation has shown promise in enhancing diagnostic precision. These models analyze subtle changes in ECG waveforms that may indicate ischemia, providing a more objective assessment compared to traditional methods. As the field advances, the integration of such technologies will be vital in addressing the complexities related to LVH and its effects on diagnosis.
Early Repolarization: Identifying ECG Features That Confuse STEMI Diagnosis
Early repolarization is characterized by J-point elevation and a concave ST-segment in the precordial leads, which can easily be mistaken for an ST-elevation myocardial infarction. This misdiagnosis is significant, as studies suggest that approximately 25% of acute myocardial infarction cases may show negative initial high-sensitivity troponin results, which can be mistaken for early repolarization. This complicates the clinical situation and emphasizes the necessity for accurate diagnosis. Developers should prioritize algorithms capable of distinguishing between early repolarization and true STEMI, as these tools are essential for improving diagnosis and outcomes for individuals.
Neural Cloud Solutions' technology exemplifies this approach. It utilizes advanced noise filtering and automated signal processing to enhance ECG interpretation. A recent study demonstrated that a machine learning model achieved a high accuracy in differentiating early repolarization from STEMI. This underscores the importance of accurate diagnosis in clinical practice.
Cardiologists stress the importance of relating ECG findings with clinical context, such as troponin levels, to ensure precise identification. As Dr. Smith notes, "It is critical to correlate ECG findings with the individual’s clinical presentation, symptoms, and additional diagnostic markers, such as troponin levels, to ensure an accurate diagnosis." The integration of advanced algorithms, like those found in MaxYield™, into clinical workflows can significantly reduce the risk of misdiagnosis, ultimately improving patient outcomes.

Ventricular Paced Rhythm: ECG Features to Differentiate from STEMI
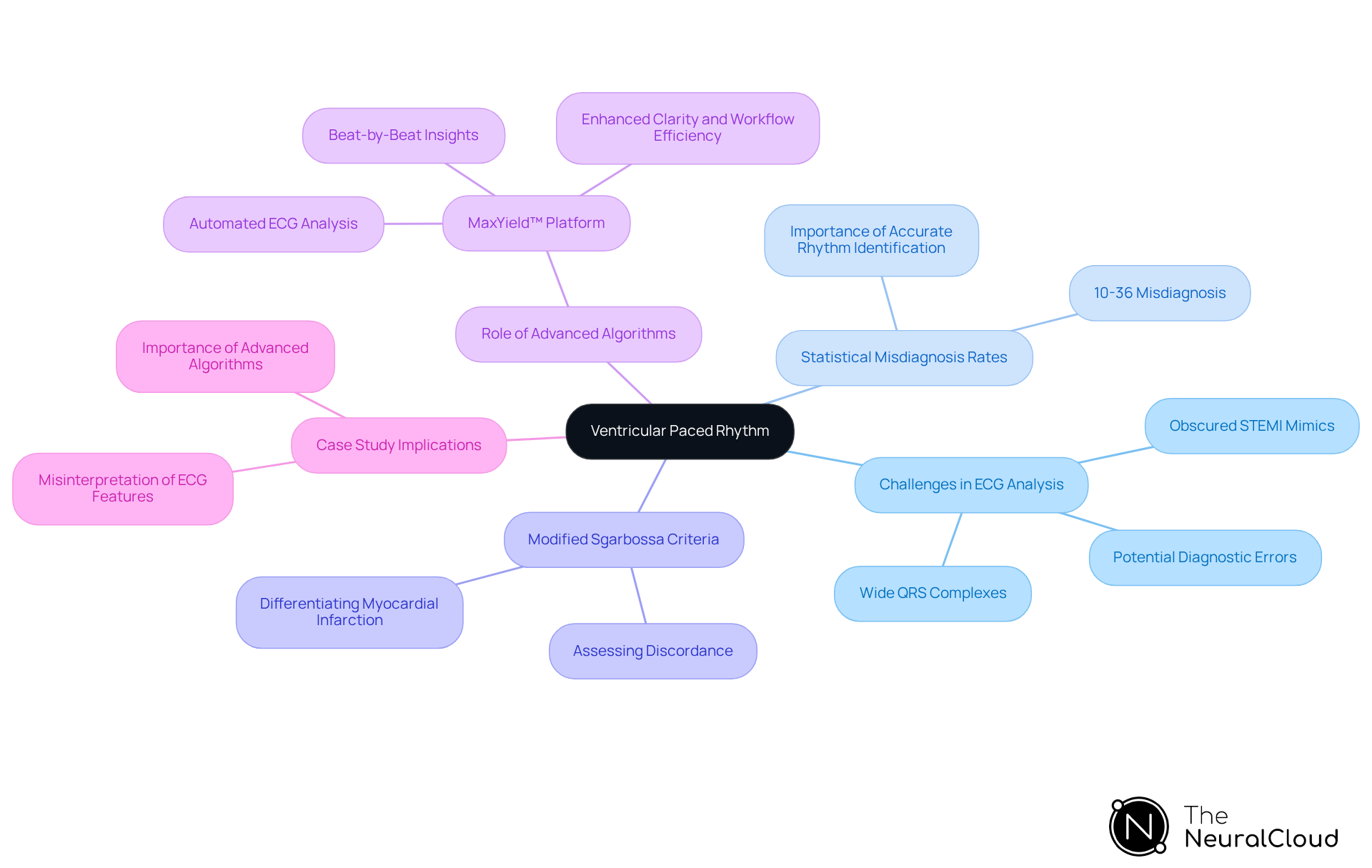
Ventricular paced rhythms present significant challenges in diagnosis, particularly due to the wide QRS complexes that can obscure classic findings of myocardial infarction, especially in the inferior leads. This masking effect complicates the interpretation of ECGs, leading to potential diagnostic errors. Studies indicate that approximately 10-36% of individuals with STEMI on ECGs do not exhibit coronary artery disease upon angiography, underscoring the necessity for accurate rhythm identification.
Healthcare professionals recognize the difficulties in diagnosing STEMI in patients who have paced rhythms. The ECG features play a crucial role in assessing discordance between the ST-segment and QRS complex, facilitating the differentiation of true myocardial infarction from baseline abnormalities associated with pacing. Algorithms designed to identify paced rhythms can significantly enhance assessment accuracy, ensuring timely and appropriate treatment.
Neural Cloud Solutions' technology effectively addresses these challenges by analyzing and providing beat-by-beat insights, analyzing 200,000 heartbeats in less than 5 minutes. This capability enables healthcare professionals to accurately identify cardiac events, even in the presence of paced rhythms. By transforming noisy recordings into detailed insights, MaxYield™ supports the detection of critical features such as P-wave, QRS complex, and T-wave intervals, thereby enhancing clarity and workflow efficiency.
Case studies illustrate that ECG features in paced rhythms can lead to misinterpretation, especially in the presence of reciprocal changes and ST elevations. The occurrence of reciprocal changes, which are ST depressions found on the opposite side of the heart from the myocardial infarction, can further complicate diagnosis. Therefore, it is essential for developers to prioritize the integration of algorithms that can accurately detect and differentiate paced rhythms, optimizing patient outcomes in emergency settings. Utilizing MaxYield™ can significantly improve diagnosis and empower healthcare professionals to make informed clinical decisions.
Hyperkalemia: ECG Indicators and Clinical Clues That Mimic STEMI
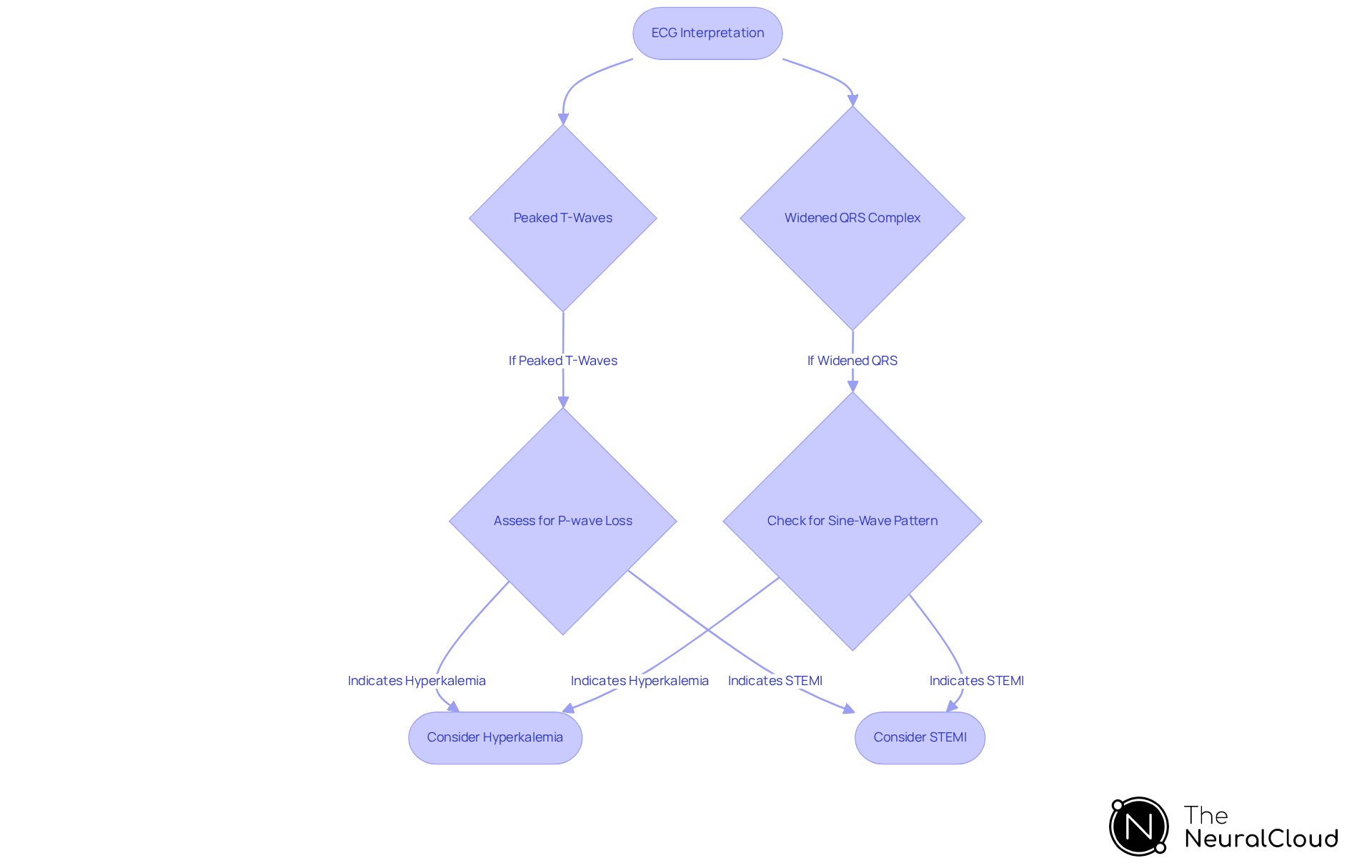
Hyperkalemia presents distinct ECG changes, such as peaked T-waves, widened QRS complexes, and potential loss of P-waves. These modifications can closely resemble stemi mimics observed in acute coronary syndrome, making precise interpretation essential. For example, hyperacute T-waves, characterized by increased height and symmetry, may be the first sign of an evolving infarct, warranting close observation. In severe cases, the QRS complex can widen significantly, leading to a sine-wave pattern that complicates diagnosis.
To address these challenges, experts emphasize the necessity for developers to incorporate algorithms capable of detecting subtle ECG changes. Neural Cloud Solutions offers advanced noise filtering and wave recognition. This technology enables the rapid isolation and labeling of critical arrhythmias, even in recordings with high levels of noise. As Daniel Kreider, MD, notes, early recognition of myocardial ischemia is crucial, as time is myocardium. Such differentiation is vital, given that studies show only approximately 43% of acute myocardial occlusions meet traditional criteria, emphasizing the need for improved diagnostic tools.
The implementation of MaxYield™, which continuously learns and enhances its algorithms, can significantly improve sensitivity in detecting STEMI mimics. By focusing on these ECG indicators and leveraging MaxYield™'s capabilities, developers can contribute to more accurate and timely diagnoses. This ultimately leads to improved patient outcomes, as healthcare professionals can make informed decisions based on precise ECG analysis.
Pulmonary Embolism: ECG Features and Clinical Signs That Mimic STEMI
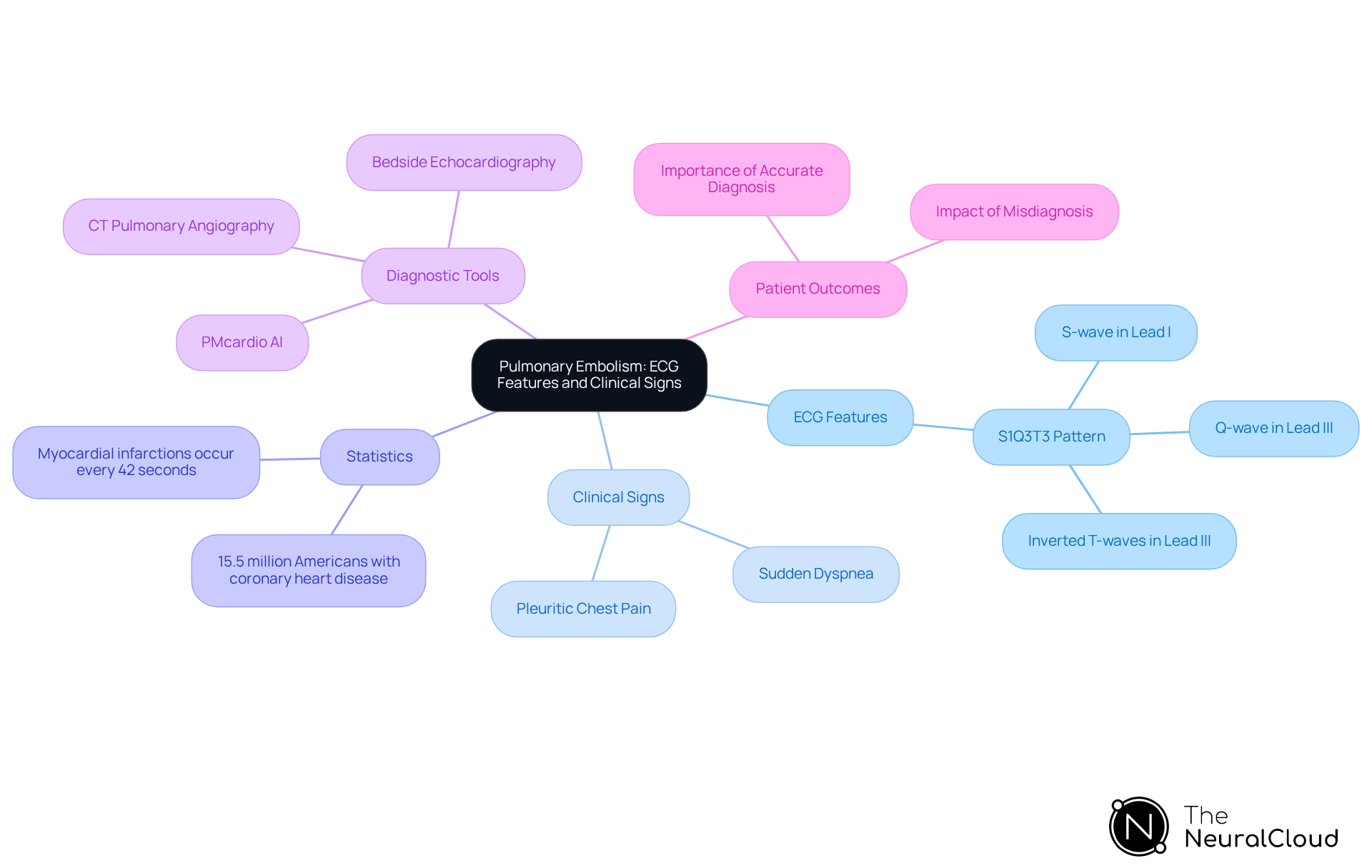
Pulmonary embolism (PE) can present with the classic S1Q3T3 pattern, which is characterized by a deep S-wave in lead I, a Q-wave in lead III, and inverted T-waves in lead III. Recognizing this unique pattern is essential for developers, as it markedly contrasts with the usual ECG results related to STEMI. Understanding these differences is crucial for developing tools capable of precisely distinguishing between PE and STEMI.
Statistics reveal that approximately 15.5 million Americans over the age of 20 suffer from PE, with events occurring every 42 seconds in the U.S. This highlights the importance of accurate ECG interpretation in emergency settings. Misdiagnosing conditions such as PE can lead to unnecessary invasive procedures and mismanagement of patient care.
Healthcare professionals stress the necessity of maintaining a high clinical suspicion when interpreting ECGs for PE. Although the classic S1Q3T3 pattern is indicative of PE, it lacks the sensitivity and specificity required to exclude STEMI. Consequently, integrating advanced diagnostic tools and imaging studies, such as CT pulmonary angiography, is vital for achieving accurate diagnoses. Neural Cloud Solutions' technology enhances this process by automating analysis, reducing noise, and providing detailed insights that assist in differentiating between these critical conditions. MaxYield™ offers beat-by-beat analysis, isolating key features in ECG signals to transform noisy recordings into actionable insights.
Real-world examples illustrate the challenges in distinguishing PE from STEMI. For instance, an individual with PE may exhibit respiratory symptoms like sudden dyspnea and pleuritic chest pain, which complicates the clinical picture. Effective communication among healthcare providers, combined with the use of advanced diagnostic tools, can enhance accuracy in assessments, ultimately improving patient outcomes in critical situations.
Advanced Diagnostics: Leveraging AI to Identify STEMI Mimics Effectively
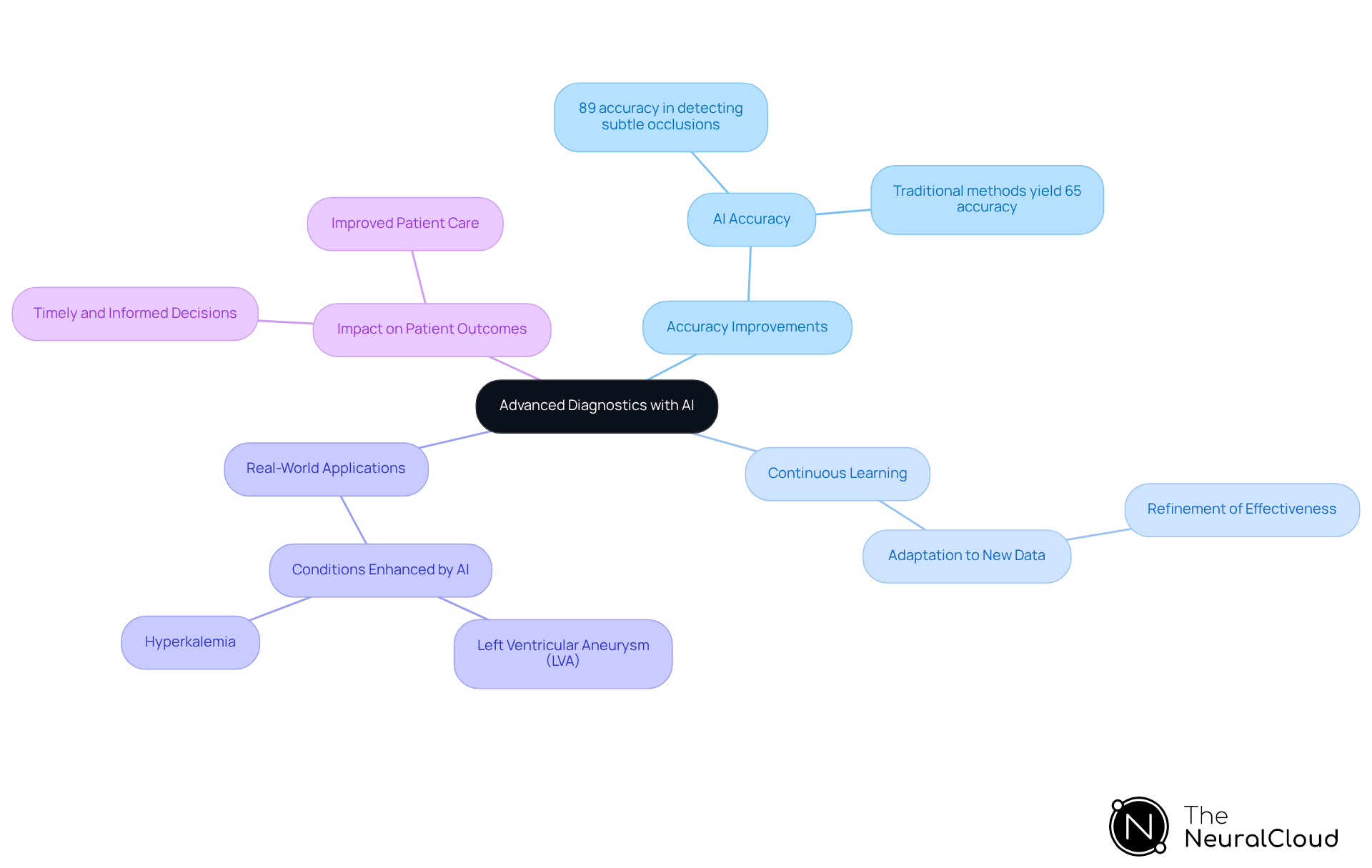
AI technologies are transforming the identification of STEMI mimics. By utilizing algorithms that analyze extensive datasets of ECG patterns, developers are creating innovative tools that significantly enhance diagnostic assessment precision and minimize the risk of misdiagnosis. Recent advancements indicate that AI can achieve an accuracy of approximately 89% in detecting STEMI mimics, surpassing traditional methods that yield around 65% accuracy. This development highlights AI's potential to revolutionize emergency medicine and improve patient outcomes.
The continuous learning capabilities of AI ensure that these assessment tools evolve, adapting to new data and refining their effectiveness over time. Experts in the field emphasize that integrating machine learning into diagnostics not only streamlines the diagnostic process but also increases the precision of distinguishing true STEMI from mimics. This distinction is particularly critical given that approximately 24-35% of patients with non-STEMI present with similar symptoms, which requires urgent intervention.
Real-world applications of these algorithms illustrate their impact on heart attack diagnosis accuracy. For instance, machine learning models have been developed that markedly enhance the identification of conditions such as left ventricular aneurysm (LVA) and hyperkalemia, which may exhibit similar ECG patterns. By leveraging advanced AI-driven solutions, healthcare professionals can make timely and informed decisions, ultimately leading to improved patient care and outcomes.
Conclusion
Understanding the various conditions that can mimic ST-Elevation Myocardial Infarction (STEMI) is crucial for healthcare professionals, particularly health tech developers. This article highlights the significance of accurately identifying these STEMI mimics, as misdiagnosis can lead to inappropriate treatments and adverse patient outcomes. Leveraging advanced technologies, such as Neural Cloud Solutions' MaxYield™ platform, significantly enhances the differentiation between genuine myocardial infarction and conditions like:
- Brugada Syndrome
- Left Bundle Branch Block
- Pericarditis
- Others
Key insights emphasize the importance of recognizing specific ECG features associated with each mimic, which can be complex and nuanced. The integration of artificial intelligence into ECG analysis is transforming how these conditions are identified, providing healthcare practitioners with the tools necessary to make informed decisions swiftly. With AI achieving superior accuracy in distinguishing between STEMI and its mimics, the potential for improved patient care is substantial.
As the landscape of health technology continues to evolve, the role of advanced diagnostic tools cannot be overstated. Developers are encouraged to focus on creating algorithms that enhance the clarity and accuracy of ECG interpretation. By doing so, they not only contribute to better clinical outcomes but also ensure that healthcare professionals are equipped to navigate the complexities of cardiac diagnostics effectively. Recognizing and addressing STEMI mimics is not just an academic exercise; it is a vital component of improving patient safety and care in emergency settings.
Frequently Asked Questions
What is Neural Cloud Solutions' MaxYield™ platform?
The MaxYield™ platform is an advanced ECG analysis tool that automates ECG signal processing and uses sophisticated AI algorithms to enhance the clarity of cardiac data, helping healthcare practitioners distinguish between genuine heart attack cases and STEMI mimics.
How does the MaxYield™ platform improve ECG analysis?
It improves ECG analysis by processing over 200,000 heartbeats in less than five minutes, allowing for rapid differentiation between myocardial infarction and STEMI mimics, ultimately leading to better clinical outcomes.
What is the significance of accurate ECG interpretation?
Accurate ECG interpretation is crucial as ongoing chest pain with ECG changes should not be ignored, even if it does not meet traditional ST-elevation MI criteria. Misinterpretation can lead to significant clinical consequences.
What is Brugada Syndrome, and how can it be mistaken for a heart attack?
Brugada Syndrome is characterized by a distinctive coved-type ST-segment elevation in the right precordial leads (V1-V3) and can often be mistaken for a heart attack. Misdiagnosis rates for STEMI mimics versus Brugada Syndrome can be as high as 30%.
How does the MaxYield™ platform assist in diagnosing Brugada Syndrome?
The MaxYield™ platform uses advanced AI-driven automation and continuous learning to analyze ECG signals, isolating and labeling key features, which enhances the accuracy of diagnosing conditions like Brugada Syndrome.
What are the key ECG indicators for Left Bundle Branch Block (LBBB)?
LBBB is characterized by a wide QRS complex (exceeding 120 ms) and an 'M' shape in leads V5 and V6. Recognizing these indicators is essential to distinguish LBBB from ST-Elevation Myocardial Infarction.
Why is it important to differentiate LBBB from myocardial infarction?
Accurate differentiation is crucial as the presence of LBBB can lead to a 2.9 times increased risk of cardiovascular mortality and complicates the identification of STEMI mimics and acute myocardial infarction.
What role does AI play in ECG analysis for STEMI mimics?
AI enhances ECG analysis by providing beat-by-beat assessments and improving diagnostic yield over time, which is essential for distinguishing between conditions like STEMI mimics, Brugada Syndrome, and LBBB.
List of Sources
- Neural Cloud Solutions: Advanced ECG Analysis for Identifying STEMI Mimics
- onlinecjc.ca (https://onlinecjc.ca/article/S0828-282X(24)00523-3/abstract)
- powerfulmedical.com (https://powerfulmedical.com/blog/may-highlights-from-powerful-medical-pmcardio-3-0-launch-stemi-research-and-clinical-breakthroughs)
- powerfulmedical.com (https://powerfulmedical.com/blog/dr-stephen-smith-discusses-the-omi-paradigm-pmcardio-on-the-parallax-podcast)
- theneuralcloud.com (https://theneuralcloud.com/post/understanding-artefact-on-ecg-types-impact-and-reduction-strategies)
- theneuralcloud.com (https://theneuralcloud.com/post/understanding-omi-meaning-significance-and-applications-in-health-tech)
- Brugada Syndrome: Recognizing ECG Features to Differentiate from STEMI
- orpha.net (https://orpha.net/en/disease/detail/130)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC5968343)
- emedicine.medscape.com (https://emedicine.medscape.com/article/163751-overview)
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- ahajournals.org (https://ahajournals.org/doi/10.1161/circep.113.000927)
- Left Bundle Branch Block (LBBB): Key ECG Indicators to Distinguish from STEMI
- STEMI Mimics: Part 2, Left Bundle Branch Block (https://practicingclinicians.com/the-exchange/stemi-mimics-part-2-left-bundle-branch-block)
- litfl.com (https://litfl.com/left-bundle-branch-block-lbbb-ecg-library)
- Left Bundle Branch Block - StatPearls - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK482167)
- Impact of Newly Diagnosed Left Bundle Branch Block on Long-Term Outcomes in Patients with STEMI (https://mdpi.com/2077-0383/13/18/5479)
- Pericarditis: Clinical Clues and ECG Features That Mimic STEMI
- ncbi.nlm.nih.gov (https://ncbi.nlm.nih.gov/books/NBK431080)
- ecgweekly.com (https://ecgweekly.com/ecgstat/criteria-findings-by-dx)
- umem.org (https://umem.org/educational_pearls/4201)
- mdpi.com (https://mdpi.com/2075-4426/12/7/1150)
- Left Ventricular Hypertrophy (LVH): ECG Characteristics That Overlap with STEMI
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- Machine learning for ECG diagnosis and risk stratification of occlusion myocardial infarction - Nature Medicine (https://nature.com/articles/s41591-023-02396-3)
- ahajournals.org (https://ahajournals.org/doi/10.1161/HYPERTENSIONAHA.119.12684)
- ahajournals.org (https://ahajournals.org/doi/10.1161/hc4201.097944)
- Early Repolarization: Identifying ECG Features That Confuse STEMI Diagnosis
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8183793)
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- Machine learning for ECG diagnosis and risk stratification of occlusion myocardial infarction - Nature Medicine (https://nature.com/articles/s41591-023-02396-3)
- ECG Patterns of Occlusion Myocardial Infarction: A Narrative Review (https://sciencedirect.com/science/article/pii/S0196064424012502)
- Ventricular Paced Rhythm: ECG Features to Differentiate from STEMI
- STEMI - Electrocardiogram - M3 Curriculum | SAEM (https://saem.org/about-saem/academies-interest-groups-affiliates2/cdem/for-students/online-education/m3-curriculum/group-electrocardiogram-(ecg)-rhythm-recognition/stemi)
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- Acute ST-Segment Elevation Myocardial Infarction (STEMI) - StatPearls - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK532281)
- ahajournals.org (https://ahajournals.org/doi/10.1161/CIRCULATIONAHA.112.104786)
- ems1.com (https://ems1.com/ems-products/medical-monitoring/articles/ecg-solution-the-right-stuff-haHqZYiGS73VwoQS)
- Hyperkalemia: ECG Indicators and Clinical Clues That Mimic STEMI
- emra.org (https://emra.org/emresident/article/stemi-equivalents)
- ems1.com (https://ems1.com/diabetes/not-your-average-sugar-rush-ems-strategies-for-dka)
- Unmasking Hyperkalemia: Highlighting Critical ECG Changes (https://powerfulmedical.com/blog/hyperkalemia-ecg-critical-changes)
- Pulmonary Embolism: ECG Features and Clinical Signs That Mimic STEMI
- medscape.com (https://medscape.com/viewarticle/quick-turn-mechanical-thrombectomy-improves-pulmonary-2025a1000cxj)
- cureus.com (https://cureus.com/articles/325992-the-crucial-role-of-bedside-echocardiography-and-clinical-suspicion-in-diagnosing-pulmonary-embolism-with-st-elevation-on-ecg-initially-misdiagnosed-as-st-segment-elevation-myocardial-infarction-stemi)
- nuemblog.com (https://nuemblog.com/blog/ecg-in-pe)
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- ECG T Wave - StatPearls - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK538264)
- Advanced Diagnostics: Leveraging AI to Identify STEMI Mimics Effectively
- Current and Future Use of Artificial Intelligence in Electrocardiography - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10145690)
- powerfulmedical.com (https://powerfulmedical.com/blog/stemi-mimics)
- Machine learning for ECG diagnosis and risk stratification of occlusion myocardial infarction - Nature Medicine (https://nature.com/articles/s41591-023-02396-3)
- Unmasking Hyperkalemia: Highlighting Critical ECG Changes (https://powerfulmedical.com/blog/hyperkalemia-ecg-critical-changes)